
Overview
-
Colleges & Schools +
- Arizona School of Dentistry & Oral Health
- Arizona School of Dentistry & Oral Health Home Page
- About Arizona School of Dentistry & Oral Health
- Admissions
- Alumni and Friends
- Community
- Faculty and Staff
- New / Current Students
- Programs
- Prospective Students
- Admissions
- Hometown Applicants
- Apply Now
- Enrollment Services
- Programs
- Student Affairs
- Housing
- Learning Resources
- Thompson Campus Center
- Still-Wellbeing Student Wellness Program
- By Campus | Kirksville/Mesa
- Online Students
- Contact Us
- University Catalog
- University Student Handbook
- LeaderScript
- Above & Beyond Award
- Student Affairs Blog
- Meet the Staff
- Enrollment Services
- University Catalog
- University Student Handbook
- Requirements
- Student Association
- Student Affairs
- Support Arizona School of Dentistry & Oral Health
- Arizona School of Dentistry & Oral Health
- Arizona School of Health Sciences
- Arizona School of Health Sciences Home Page
- About Arizona School of Health Sciences
- Admissions
- Alumni and Friends
- Faculty and Staff
- New/Current Students
- Departments
- Online Programs
- Doctor of Athletic Training (DAT)
- Doctor of Medical Science
- Post-Professional Doctor of Audiology
- Post-Professional Doctor of Physical Therapy
- Post-Professional Doctor of Physical Therapy - non-degree
- Post-Professional Doctor of Audiology - non-degree
- Master of Science in Biomedical Sciences
- Canvas Demo Course
- Campus Based Programs
- Certificate Programs
- Graduate Certificate in Clinical Decision-Making in Athletic Training
- Graduate Certificate in Orthopaedics
- Graduate Certificate in Rehabilitation
- Graduate Certificate in Leadership and Education
- Graduate Certificate in Sport Neurology and Concussion
- Certificate in Public Health, Emergency Preparedness & Disaster Response
- Certificate in Health Professions Education
- Certificate in Adaptive Sports
- Certificate in Corrective Exercise & Orthopedic Rehabilitation
- Certificate in Exercise and Sport Psychology
- Certificate in Geriatric Exercise Science
- Certificate in Sports Conditioning
- Certificate in Fundamentals of Education
- Certificate in Global Health Concentration
- Certificate in Leadership & Organizational Behavior
- Prospective Students
- Residential Programs
- Student Affairs
- Support Arizona School of Health Sciences
- College of Graduate Health Studies
- College of Graduate Health Studies Home Page
- About College of Graduate Health Studies
- Admissions
- Alumni and Friends
- Commitment and Values
- Faculty & Staff
- Mission
- New / Current Students
- Programs
- Request Information
- Contact a Representative
- Apply Now
- Doctor of Health Administration
- a href="/college-of-graduate-health-studies/academics/doctor-of-health-sciences-degree-online">Doctor of Health Sciences
- Doctor of Nursing Practice
- Master of Health Administration
- Master of Public Health
- Master of Public Health - Dental Emphasis
- Master of Public Health - Dental Emphasis with a Dental Public Health Residency Certificate
- Master of Science in Kinesiology
- Canvas Demo Course
- Prospective Students
- Student Affairs
- Support College of Graduate Health Studies
- College for Healthy Communities
- Kirksville College of Osteopathic Medicine
- Kirksville College of Osteopathic Medicine Home Page
- About Kirksville College of Osteopathic Medicine
- Admissions
- Alumni & Friends
- Continuing Education (CE)
- Faculty & Staff
- New/Current Students
- New and Current Student Home
- Accepted Students
- Kirksville College of Osteopathic Medicine Academic Calendar
- Student Affairs
- Enrollment Services
- Academic Affairs
- Clinical Rotations
- Kirksville College of Osteopathic Medicine-AHEC Program
- Preceptor Information
- Postdoctoral Study (Still OPTI)
- Scholarly Activity
- ATSU Portal
- Kirksville College of Osteopathic Medicine Graduation
- University Student Handbook
- Kirksville College of Osteopathic Medicine Catalog
- Programs
- Prospective Students
- Prospective Student Home
- Kirksville College of Osteopathic Medicine Academic Calendar
- Admissions
- Application Process
- Premedical Student Checklist
- Top Ten Application Mistakes
- Personal Statement Tips
- Ambassadors
- Apply Now
- Enrollment Services
- Programs
- Student Affairs
- Kirksville College of Osteopathic Medicine Catalog
- Visit the Museum
- Board Scores
- Postgraduate Placement
- University Catalog
- University Student Handbook
- Student Affairs
- Support Kirksville College of Osteopathic Medicine
- Missouri School of Dentistry & Oral Health
- School of Osteopathic Medicine Arizona
- School of Osteopathic Medicine in Arizona Home Page
- About School of Osteopathic Medicine in Arizona
- Academics
- Admissions
- Alumni and Friends
- Faculty & Staff
- New / Current Students
- Accepted Students
- Student Services
- Enrollment Services
- Academic Affairs
- Clinical Rotations
- ATSU Portal
- University Student Handbook
- School of Osteopathic Medicine in Arizona Academic Calendars
- Graduation
- Programs
- Prospective Students
- Student Affairs
- Osteopathic Medicine Center
- Support School of Osteopathic Medicine in Arizona
Looking for This +
- About ATSU
- Programs of Study
- Residential Programs
- Doctorate Level Degree Programs
- Doctor of Audiology (AuD)
- Doctor of Dental Medicine - AZ (DMD)
- Doctor of Dental Medicine - MO (DMD)
- Occupational Therapy Entry-level - AZ (OTD-E)
- Doctor of Physical Therapy (DPT)
- Doctor of Health Sciences (DHSc)
- Doctor of Occupational Therapy - Entry Level
- Doctor of Osteopathic Medicine - AZ (DO)
- Doctor of Osteopathic Medicine - MO (DO)
- Master's in Orthodontics
- Master Level Degree Programs
- Doctorate Level Degree Programs
- Online Programs
- Doctorate Level Degree Programs
- Masters Level Degree Programs
- Advanced Physician Assistant (APA)
- Master of Health Administration (MHA)
- Master of Public Health Policy (MPH)
- Master of Public Health - Dental Emphasis (MPH-DE)
- Master of Public Health - Dental Emphasis with a Dental Public Health Residency Certificate
- Master of Science in Kinesiology
- Master of Education in Health Professions Education (MEd)
- Master of Health Sciences (MHSc)
- Residency programs
- Online/Residential Blend Programs
- Continuing Education - CME
- Research
- Certificate Programs
- Graduate Certificate in Clinical Decision-Making in Athletic Training
- Graduate Certificate in Orthopaedics
- Graduate Certificate in Rehabilitation
- Graduate Certificate in Leadership and Education
- Graduate Certificate in Sport Neurology and Concussion
- Certificate in Public Health, Emergency Preparedness & Disaster Response
- Certificate in Health Professions Education
- Certificate in Adaptive Sports
- Certificate in Corrective Exercise & Orthopedic Rehabilitation
- Certificate in Exercise and Sport Psychology
- Certificate in Geriatric Exercise Science
- Certificate in Sports Conditioning
- Certificate in Fundamentals of Education
- Certificate in Global Health Concentration
- Certificate in Leadership & Organizational Behavior
- Request Information
- Contact a Representative
- Apply Now
- Request a Tour
- Residential Programs
- Tuition
- Institutional Effectiveness
- Catalog
- Colleges & Schools
- Arizona School of Dentistry & Oral Health (ASDOH)
- Arizona School of Health Sciences (ASHS)
- College of Graduate Health Studies (CGHS)
- CGHS Home Page
- Doctor of Health Education (DHEd)
- Doctor of Health Administration (DHA)
- Doctor of Health Sciences (DHSc)
- Master of Health Administration (MHA)
- Master of Public Health (MPH)
- Master of Public Health – Dental Emphasis
- Master of Public Health - Dental Emphasis with a Dental Public Health Residency Certificate
- Master of Science in Kinesiology
- Kirksville College of Osteopathic Medicine (KCOM)
- Missouri School of Dentistry & Oral Health (MOSDOH)
- School of Osteopathic Medicine in Arizona (SOMA)
- ASHS Departments
- Facilities and Clinics
- Research
- Get Involved
- Clinical Experience Sites
- Student Affairs
- Admissions
- Enrollment Services
- Student Life
- Housing
- Learning Resources and Counseling
- Wellness Programs
- Thompson Campus Center
- National Center for Native American Indian Health Professions
I Want To +
- Connect
- Learn
- About ATSU
- Osteopathic Medicine DO (Residential)
- Biomedical Sciences (MS)
- Audiology (AuD)
- Physical Therapy Orthopedic Residency
- Neurologic Physical Therapy Residency
- Doctor of Athletic Training (DAT)
- Doctor of Medical Science
- Athletic Training (MS)
- Occupational Therapy Entry-level (OTD-E)
- Master of Science in Occupational Therapy
- Physician Assistant Studies (MS)
- Doctor of Health Sciences (DHSc)
- Post-Professional Doctor of Audiology (AuD)
- Post-Professional Doctor of Physical Therapy (DPT)
- Post-Professional Physical Therapy - non-degree
- Master of Science in Kinesiology
- Doctor of Health Education (DHEd)
- Health Administration (MHA)
- Public Health (MPH)
- Master of Public Health - Dental Emphasis (MPH)
- Master of Public Health - Dental Emphasis with a Dental Public Health Residency Certificate
- Dental Medicine (DMD) - Missouri campus
- Certificate in Clinical Decision-Making in Athletic Training
- Certificate in Leadership and Organizational Behavior, Doctor of Health Sciences
- Certificate in Global Health, Doctor of Health Sciences
- Certificate in Fundamentals of Education, Doctor of Health Sciences
- Graduate Certificate in Orthopedic Rehabilitation
- Master's in Orthodontics
- Discover
- Complete & Fill Out
- Support ATSU
- Apply
- Look-Up
- Locate
- Contact
ATSU Portal Login
Overview
-
Colleges & Schools +
- Arizona School of Dentistry & Oral Health
- Arizona School of Dentistry & Oral Health Home Page
- About Arizona School of Dentistry & Oral Health
- Admissions
- Alumni and Friends
- Community
- Faculty and Staff
- New / Current Students
- Programs
- Prospective Students
- Admissions
- Hometown Applicants
- Apply Now
- Enrollment Services
- Programs
- Student Affairs
- Housing
- Learning Resources
- Thompson Campus Center
- Still-Wellbeing Student Wellness Program
- By Campus | Kirksville/Mesa
- Online Students
- Contact Us
- University Catalog
- University Student Handbook
- LeaderScript
- Above & Beyond Award
- Student Affairs Blog
- Meet the Staff
- Enrollment Services
- University Catalog
- University Student Handbook
- Requirements
- Student Association
- Student Affairs
- Support Arizona School of Dentistry & Oral Health
- Arizona School of Dentistry & Oral Health
- Arizona School of Health Sciences
- Arizona School of Health Sciences Home Page
- About Arizona School of Health Sciences
- Admissions
- Alumni and Friends
- Faculty and Staff
- New/Current Students
- Departments
- Online Programs
- Doctor of Athletic Training (DAT)
- Doctor of Medical Science
- Post-Professional Doctor of Audiology
- Post-Professional Doctor of Physical Therapy
- Post-Professional Doctor of Physical Therapy - non-degree
- Post-Professional Doctor of Audiology - non-degree
- Master of Science in Biomedical Sciences
- Canvas Demo Course
- Campus Based Programs
- Certificate Programs
- Graduate Certificate in Clinical Decision-Making in Athletic Training
- Graduate Certificate in Orthopaedics
- Graduate Certificate in Rehabilitation
- Graduate Certificate in Leadership and Education
- Graduate Certificate in Sport Neurology and Concussion
- Certificate in Public Health, Emergency Preparedness & Disaster Response
- Certificate in Health Professions Education
- Certificate in Adaptive Sports
- Certificate in Corrective Exercise & Orthopedic Rehabilitation
- Certificate in Exercise and Sport Psychology
- Certificate in Geriatric Exercise Science
- Certificate in Sports Conditioning
- Certificate in Fundamentals of Education
- Certificate in Global Health Concentration
- Certificate in Leadership & Organizational Behavior
- Prospective Students
- Residential Programs
- Student Affairs
- Support Arizona School of Health Sciences
- College of Graduate Health Studies
- College of Graduate Health Studies Home Page
- About College of Graduate Health Studies
- Admissions
- Alumni and Friends
- Commitment and Values
- Faculty & Staff
- Mission
- New / Current Students
- Programs
- Request Information
- Contact a Representative
- Apply Now
- Doctor of Health Administration
- a href="/college-of-graduate-health-studies/academics/doctor-of-health-sciences-degree-online">Doctor of Health Sciences
- Doctor of Nursing Practice
- Master of Health Administration
- Master of Public Health
- Master of Public Health - Dental Emphasis
- Master of Public Health - Dental Emphasis with a Dental Public Health Residency Certificate
- Master of Science in Kinesiology
- Canvas Demo Course
- Prospective Students
- Student Affairs
- Support College of Graduate Health Studies
- College for Healthy Communities
- Kirksville College of Osteopathic Medicine
- Kirksville College of Osteopathic Medicine Home Page
- About Kirksville College of Osteopathic Medicine
- Admissions
- Alumni & Friends
- Continuing Education (CE)
- Faculty & Staff
- New/Current Students
- New and Current Student Home
- Accepted Students
- Kirksville College of Osteopathic Medicine Academic Calendar
- Student Affairs
- Enrollment Services
- Academic Affairs
- Clinical Rotations
- Kirksville College of Osteopathic Medicine-AHEC Program
- Preceptor Information
- Postdoctoral Study (Still OPTI)
- Scholarly Activity
- ATSU Portal
- Kirksville College of Osteopathic Medicine Graduation
- University Student Handbook
- Kirksville College of Osteopathic Medicine Catalog
- Programs
- Prospective Students
- Prospective Student Home
- Kirksville College of Osteopathic Medicine Academic Calendar
- Admissions
- Application Process
- Premedical Student Checklist
- Top Ten Application Mistakes
- Personal Statement Tips
- Ambassadors
- Apply Now
- Enrollment Services
- Programs
- Student Affairs
- Kirksville College of Osteopathic Medicine Catalog
- Visit the Museum
- Board Scores
- Postgraduate Placement
- University Catalog
- University Student Handbook
- Student Affairs
- Support Kirksville College of Osteopathic Medicine
- Missouri School of Dentistry & Oral Health
- School of Osteopathic Medicine Arizona
- School of Osteopathic Medicine in Arizona Home Page
- About School of Osteopathic Medicine in Arizona
- Academics
- Admissions
- Alumni and Friends
- Faculty & Staff
- New / Current Students
- Accepted Students
- Student Services
- Enrollment Services
- Academic Affairs
- Clinical Rotations
- ATSU Portal
- University Student Handbook
- School of Osteopathic Medicine in Arizona Academic Calendars
- Graduation
- Programs
- Prospective Students
- Student Affairs
- Osteopathic Medicine Center
- Support School of Osteopathic Medicine in Arizona
Looking for This +
- About ATSU
- Programs of Study
- Residential Programs
- Doctorate Level Degree Programs
- Doctor of Audiology (AuD)
- Doctor of Dental Medicine - AZ (DMD)
- Doctor of Dental Medicine - MO (DMD)
- Occupational Therapy Entry-level - AZ (OTD-E)
- Doctor of Physical Therapy (DPT)
- Doctor of Health Sciences (DHSc)
- Doctor of Occupational Therapy - Entry Level
- Doctor of Osteopathic Medicine - AZ (DO)
- Doctor of Osteopathic Medicine - MO (DO)
- Master's in Orthodontics
- Master Level Degree Programs
- Doctorate Level Degree Programs
- Online Programs
- Doctorate Level Degree Programs
- Masters Level Degree Programs
- Advanced Physician Assistant (APA)
- Master of Health Administration (MHA)
- Master of Public Health Policy (MPH)
- Master of Public Health - Dental Emphasis (MPH-DE)
- Master of Public Health - Dental Emphasis with a Dental Public Health Residency Certificate
- Master of Science in Kinesiology
- Master of Education in Health Professions Education (MEd)
- Master of Health Sciences (MHSc)
- Residency programs
- Online/Residential Blend Programs
- Continuing Education - CME
- Research
- Certificate Programs
- Graduate Certificate in Clinical Decision-Making in Athletic Training
- Graduate Certificate in Orthopaedics
- Graduate Certificate in Rehabilitation
- Graduate Certificate in Leadership and Education
- Graduate Certificate in Sport Neurology and Concussion
- Certificate in Public Health, Emergency Preparedness & Disaster Response
- Certificate in Health Professions Education
- Certificate in Adaptive Sports
- Certificate in Corrective Exercise & Orthopedic Rehabilitation
- Certificate in Exercise and Sport Psychology
- Certificate in Geriatric Exercise Science
- Certificate in Sports Conditioning
- Certificate in Fundamentals of Education
- Certificate in Global Health Concentration
- Certificate in Leadership & Organizational Behavior
- Request Information
- Contact a Representative
- Apply Now
- Request a Tour
- Residential Programs
- Tuition
- Institutional Effectiveness
- Catalog
- Colleges & Schools
- Arizona School of Dentistry & Oral Health (ASDOH)
- Arizona School of Health Sciences (ASHS)
- College of Graduate Health Studies (CGHS)
- CGHS Home Page
- Doctor of Health Education (DHEd)
- Doctor of Health Administration (DHA)
- Doctor of Health Sciences (DHSc)
- Master of Health Administration (MHA)
- Master of Public Health (MPH)
- Master of Public Health – Dental Emphasis
- Master of Public Health - Dental Emphasis with a Dental Public Health Residency Certificate
- Master of Science in Kinesiology
- Kirksville College of Osteopathic Medicine (KCOM)
- Missouri School of Dentistry & Oral Health (MOSDOH)
- School of Osteopathic Medicine in Arizona (SOMA)
- ASHS Departments
- Facilities and Clinics
- Research
- Get Involved
- Clinical Experience Sites
- Student Affairs
- Admissions
- Enrollment Services
- Student Life
- Housing
- Learning Resources and Counseling
- Wellness Programs
- Thompson Campus Center
- National Center for Native American Indian Health Professions
I Want To +
- Connect
- Learn
- About ATSU
- Osteopathic Medicine DO (Residential)
- Biomedical Sciences (MS)
- Audiology (AuD)
- Physical Therapy Orthopedic Residency
- Neurologic Physical Therapy Residency
- Doctor of Athletic Training (DAT)
- Doctor of Medical Science
- Athletic Training (MS)
- Occupational Therapy Entry-level (OTD-E)
- Master of Science in Occupational Therapy
- Physician Assistant Studies (MS)
- Doctor of Health Sciences (DHSc)
- Post-Professional Doctor of Audiology (AuD)
- Post-Professional Doctor of Physical Therapy (DPT)
- Post-Professional Physical Therapy - non-degree
- Master of Science in Kinesiology
- Doctor of Health Education (DHEd)
- Health Administration (MHA)
- Public Health (MPH)
- Master of Public Health - Dental Emphasis (MPH)
- Master of Public Health - Dental Emphasis with a Dental Public Health Residency Certificate
- Dental Medicine (DMD) - Missouri campus
- Certificate in Clinical Decision-Making in Athletic Training
- Certificate in Leadership and Organizational Behavior, Doctor of Health Sciences
- Certificate in Global Health, Doctor of Health Sciences
- Certificate in Fundamentals of Education, Doctor of Health Sciences
- Graduate Certificate in Orthopedic Rehabilitation
- Master's in Orthodontics
- Discover
- Complete & Fill Out
- Support ATSU
- Apply
- Look-Up
- Locate
- Contact
ATSU Portal Login
Interprofessional Education
When it comes to thinking about creating interprofessional curricula for pre-registration students, Barr and Low (2012) describe the need to create “outcome-led competency-based interprofessional curricula grounded in coherent, theoretical rationale, while safeguarding the identity of each profession and respecting profession-specific requirements and benchmarking statements.”
Definitions:
Interprofessional Education: “Those occasions when members of two or more professions learn with, from, and about one another to improve collaboration and the quality of [service].” (CAIPE 1997)
Interprofessional Collaborative Practice: “When multiple health workers from different professional backgrounds work together with patients, families, careers, and communities to deliver the highest quality of care.” (WHO, 2010)
Interprofessionality: “An education and practice orientation, an approach to care and education where educators and practitioners collaborate synergistically.” (d’Amour and Oandasan 2005 p10)
Theory +
-
Theories applied to interprofessional education
Interprofessional education and collaborative practice have borrowed heavily and widely from various academies of thought, including sociology, psychology, education, anthropology, economics, political science, organizational theory…... and so on. The aim of this section is to present a synopsis of the relevant theories espoused in relation to interprofessional education and bring together a wide array of resources for those who wish to dive a little deeper.
Some authors have already attempted to draw together and condense some of this work, below are some papers worth reading if you want a good overview of some diverse, though mostly sociological theory as applied to inter professional education
The Theory Practice Relationship in Interprofessional Education
Theoretical Insights into Interprofessional Education: AMEE Guide No.62
Clark PG. What would a theory of interprofessional education look like? Some suggestions for developing a theoretical framework for teamwork training 1. J Interprof Care. 2006 Dec;20(6):577-89. PubMed PMID: 17095437.
The focus of the January 2013 edition of the Journal of Interprofessional Care (Volume 27), was theory use in interprofessional education and collaboration.For a Deeper Exploration of Individual Theories
You may wish to consider the following theories. This list is not exhaustive.
Sociological Theories
- Theories of Social Action
- Social Capital Theory
- Contact Hypothesis
- Activity Theory
- Complexity Theory
- Stereotyping
- Social Identity Theory
- Generalization
Psychological Theories
- Group Work and Teamwork Approaches
- Attitude change
- Factors that Mediate Behavioral Change
Adult Learning Theories
- Problem-based learning
- Situational Learning and Communities of Practice
-
Outcome Measures +
-
The National Center for Interprofessional Practice and Education - Assessment Help and Tools
Assessment Help
Tool RepositoryCIHC Evaluation Framework
The CIHC Evaluation Framework originated from the interprofessional education for collaborative, patient-centred practice projects (IECPCP), funded by Health Canada. The initial intent was to catalog the instruments and outcomes of the funded projects. Further development by D’Amour and Oandasan (2004) has led to the provision of this very useful resource that can assist with the selection of assessment tools for interprofessional activities, including assessment of the educational system, health professional learner outcomes, the professional system, government policy, and patient / provider outcomes.
Example Published / Validated Instruments
- ATHT - Attitudes Towards Health Care Teams
- iCCAS - The Interprofessional Collaborative Competency Attainment Scale
- ITPS - Interprofessional Team Performance Scale
- IEPS - Interdisciplinary Education Perception Scale
- IPRQ - Interprofessional Reciprocity Pre-Questionnaire
- CSCD - Collaboration and Satisfaction about Care Decisions Scale
Best Practice Guidelines and Reviews
The following articles contain reviews and guidelines on how to apply best practice to the evaluation of interprofessional educational activities.
- Freeth, D., Reeves, S., Koppel, I., Hammick, M., Barr, H. (2005) Evaluating Interprofessional Education: A Self-Help Guide. Higher Education Academy.
This article by Freeth et al (2005) provides a guide for both novice and experienced evaluators to assessing interprofessional activities. It includes the 3P model adapted from Freeth & Reeves (2004), the 3P’s representing presage, process and product. Presage relates to the constraints and influences on the design and delivery of IPE activities, process to the delivery, including approaches to teaching and learning, and product is concerned with the outcomes of IPE activities.
This article catalogs the evaluation frameworks and tools used in 20 Canadian interprofessianal education and collaborative patient-centered practice (IECPCP) learning projects.
- Thistlethwaite J, Moran M; World Health Organization Study Group on Interprofessional Education and Collaborative Practice. Learning Outcomes for Interprofessional Education : Literature Review and Synthesis. J Interprof Care. 2010 Sep;24(5):503-13. Review. PubMed PMID: 20718596.
- Gillan C, Lovrics E, Halpern E, Wiljer D, Harnett N. The evaluation of learner outcomes in interprofessional continuing education: a literature review and an analysis of survey instruments. Med Teach. 2011;33(9):e461-70. Review. PubMed PMID: 21854139.
The following articles relate to specific measurement tools
ATHT - Attitudes Towards Health Care Teams- Heinemann, G.D., Schmitt, M.H., Farrell, M.P., & Brallier, S.A. (1999). Development of an Attitudes Toward Health Care Teams Scale. Evaluation & the Health Professions, 22, 123-142.
- Hyer, K., Fairchild, S., Abraham, I., Mezey, M., Fulmer, T. (2000). Measuring attitudes related to interdisciplinary training: revisiting the Heinemann, Schmitt and Farrell ‘attitudes toward health care teams’ scale Journal of Interprofessional Care 14(3): 249-258.
RIPLS - Readiness for Interprofessional Learning Scale
- Parsell G, Bligh J. The development of a questionnaire to assess the readiness of health care students for interprofessional learning (RIPLS). Med Educ. 1999 Feb;33(2):95-100. PubMed PMID: 10211258.
- McFadyen, A.K., Webster V., Strachan K., Figgins E., Brown H., Mckechnie J. (2005). The Readiness for interprofessional learning scale: A possible more stable sub-scale model for the original version of RIPLS. Journal of Interprofessional Care 19(6): 595 – 603.
ITPS - Interprofessional Team Performance Scale
IEPS - Interdisciplinary Education Perception Scale
- Luecht RM, Madsen MK, Taugher MP, Petterson BJ. (1990). Assessing professional perceptions: design and validation of an Interdisciplinary Education Perception Scale. Journal of Allied Health 19(2):181-91
IPRQ - Interprofessional Reciprocity Pre-Questionnaire
CSCD - Collaboration and Satisfaction about Care Decisions Scale
- Lê Q, Spencer J, Whelan J. Development of a tool to evaluate health science students’ experiences of an interprofessional education (IPE) programme. Ann Acad Med Singapore. 2008 Dec;37(12):1027-33. PubMed PMID: 19159037.
-
Evidence IPE +
-
Interprofessional Journals
Journal of Interprofessional Care
Journal of Research in Interprofessional Practice and EducationReviews and Systematic Reviews
- Hammick M., Freeth D., Koppel I., Reeves S., and Barr H., A Best Evidence Systematic Review of Interprofessional Education: BEME Guide no. 9, Medical Teacher, 2007, 29(8): 735-751.
- Cooper H., Carlisle C., Watkins C., Gibbs T. 2001 Developing an evidence base for interdisciplinary learning, Journal of Advanced Nursing, 35 92):228-237
- Reeves S, Zwarenstein M, Goldman J, Barr H, Freeth D, Koppel I, Hammick M. The effectiveness of interprofessional education: key findings from a new systematic review. J Interprof Care. 2010 May;24(3):230-41. Review. PubMed PMID: 20178425.
- Reeves S, Zwarenstein M, Goldman J, Barr H, Freeth D, Hammick M, Koppel I., Interprofessional education: effects on professional practice and health care outcomes. Cochrane Database Syst Rev. 2008 Jan 23;(1):CD002213. Review. PubMed PMID: 18254002.
- Thistlethwaite J. Interprofessional education: a review of context, learning and the research agenda. Med Educ. 2012 Jan;46(1):58-70. doi:10.1111/j.1365-2923.2011.04143.x. PubMed PMID: 22150197.
Making Interprofessional Education Work
- Oandasan I. and Reeves S., Key Elements of Interprofessional Education. Part 1: The Learner, the Educator, and the Learning Context, Journal of Interprofessional Care, May 2005, 1 (suppl): 21-38.
- Oandasan I. and Reeves S., Key Elements of Interprofessional Education. Part 2: Factors, Processes and Outcomes, Journal of Interprofessional Care, May 2005, 1 (suppl): 39-48.
- Reeves S, Goldman J, Oandasan I. Key factors in planning and implementing interprofessional education in health care settings. J Allied Health. 2007 Winter;36(4):231-5. PubMed PMID: 18293805.
- Thistlethwaite J, Moran M; World Health Organization Study Group on Interprofessional Education and Collaborative Practice. Learning outcomes for interprofessional education (IPE): Literature review and synthesis. J Interprof Care. 2010 Sep;24(5):503-13. Review. PubMed PMID: 20718596.
- Kendall H., et al., Making Interprofessional Education Work: The Strategic Roles of the Academy, Academic Medicine, October 2008, 83(10): 934-940.
- Bridges DR, Davidson RA, Odegard PS, Maki IV, Tomkowiak J. Interprofessional collaboration: three best practice models of interprofessional education. Med Educ Online. 2011 Apr 8;16. doi: 10.3402/meo.v16i0.6035. PubMed PMID: 21519399; PubMed Central PMCID: PMC3081249.
- Hoffman SJ, Harnish D. The merit of mandatory interprofessional education for pre-health professional students. Med Teach. 2007 Oct;29(8):e235-42. PubMed PMID: 18236267.
- Buring SM, Bhushan A, Broeseker A, Conway S, Duncan-Hewitt W, Hansen L, Westberg S. Interprofessional education: definitions, student competencies, and guidelines for implementation. Am J Pharm Educ. 2009 Jul 10;73(4):59. PubMed. PMID: 19657492; PubMed Central PMCID: PMC2720355.
Faculty Development
- Curran VR, Deacon DR, Fleet L. Academic administrators’ attitudes towards interprofessional education in Canadian schools of health professional education. J Interprof Care. 2005 May;19 Suppl 1:76-86. PubMed PMID: 16096147.
- Curran V.R., Sharpe D., and Forristall J., Attitudes of Health Sciences Faculty Members Towards Interprofessional Education, Medical Education, 2007, 41: 892-896.
- Alberto J., Herth K., Interprofessional Collaboration within Faculty Roles: Teaching, Service and Research. Online Journal of Issues in Nursing, 2009, May:14 (2).
- Silver I.L. and Leslie K., Faculty Development for Continuing Interprofessional Education and Collaborative Practice, Journal of Continuing Education in the Health Professions, 2009, 29(3): 172-177. PubMed PMID: 19728382.
- Steinert Y. Learning Together to Teach Together: Interprofessional Education and Faculty Development, Journal of Interprofessional Care, May 2005, Supplement 1: 60-75. PubMed PMID: 1609614
- Ho K, Jarvis-Selinger S, Borduas F, Frank B, Hall P, Handfield-Jones R, Hardwick DF, Lockyer J, Sinclair D, Lauscher HN, Ferdinands L, MacLeod A, Robitaille MA, Rouleau M. Making interprofessional education work: the strategic roles of the academy. Acad Med. 2008 Oct;83(10):934-40. Review. PubMed PMID: 18820523
- Egan-Lee E, Baker L, Tobin S, Hollenberg E, Dematteo D, Reeves S. Neophyte facilitator experiences of interprofessional education: implications for faculty development. J Interprof Care. 2011 Sep;25(5):333-8. PubMed PMID: 21823882.
Pre-registration Students
- Johnson AW, Potthoff SJ, Carranza L, Swenson HM, Platt CR, Rathbun JR. CLARION: a novel interprofessional approach to health care education. Acad Med. 2006 Mar;81(3):252-6. PubMed PMID: 16501268.
- Moray House Study (McMichael & Gilloram, 1984)
- The Bristol Studies (Carpenter & Hewstone
- Curran V.R., Sharpe D., Flynn K., and Button P., A Longitudinal Study of the Effect of an Interprofessional Education Curriculum on Student Satisfaction and Attitudes Towards Interprofessional Teamwork and Education, Journal of Interprofessional Care, January 2010, 24(1): 41-52.
- Hawk C., Buckwalter K., Byrd L., Cigelman S., Dorfman L., and Ferguson K., Health Professions Students’ Perceptions of Interprofessional Relationships, Academic Medicine, April 2002, 77(4): 354-357.
- Reeves S. and Pryce A., Emerging themes: an exploratory research project of an interprofessional education module for medical, dental and nursing students, Nurse Education Today, October 1998, 18(7): 534-541.
- Solomon P., Baptiste S., Hall P., Luke R., Orchard C., Rukholm E., Carter L., King S., and Damiani-Taraba G., Students’ Perceptions of Interprofessional Learning Through Facilitated Online Learning Modules, Medical Teacher, 2010, 32: e391-e398.
- Hall,P.D., Zoller, J.S., West V.T., Lancaster, C.J., Blue A.V. A Novel Approach to Interprofessional Education: Interprofessional Day, the Four-Year Experience at the Medical University of South Carolina. Journal of Research in Interprofessional Practice and Education Vol. 2.1 July, 2011
- Coster S, Norman I, Murrells T, Kitchen S, Meerabeau E, Sooboodoo E, d’Avray L., Interprofessional attitudes amongst undergraduate students in the health professions: a longitudinal questionnaire survey. Int J Nurs Stud. 2008 Nov;45(11):1667-81. Epub 2008 Apr 18. PubMed PMID: 18423644.
- Cooper H, Spencer-Dawe E, McLean E. Beginning the process of teamwork: design, implementation and evaluation of an inter-professional education intervention for first year undergraduate students. J Interprof Care. 2005 Oct;19(5):492-508. PubMed PMID: 16308172.
- Pollard KC, Miers ME. From students to professionals: results of a longitudinal study of attitudes to pre-qualifying collaborative learning and working in health and social care in the United Kingdom. J Interprof Care. 2008 Aug;22(4):399-416. PubMed PMID: 18800281.
- Pollard KC, Miers ME, Gilchrist M, Sayers A. A comparison of interprofessional perceptions and working relationships among health and social care students: the results of a 3-year intervention. Health Soc Care Community. 2006 Nov;14(6):541-52. PubMed PMID: 17059496.
Post-Professional Students
- The Birmingham Study (Barnes et al, 2000)
-
Evidence ICP +
-
Systematic Reviews
- Zwarenstein M., Goldman J., and Reeves S., Interprofessional Collaboration: Effects of Practice-Based Interventions on Professional Practice and Healthcare Outcomes (Review), Cochrane Database of Systematic Reviews 2009, Issue 3. Art No: CD000072 DOI: 10.1002/14651858.CD000072pub2.
- Reeves S, Zwarenstein M, Goldman J, Barr H, Freeth D, Hammick M, Koppel I., Interprofessional education: effects on professional practice and health care outcomes. Cochrane Database Syst Rev. 2008 Jan 23;(1):CD002213. Review. PubMed PMID: 18254002.
Practice-based Education
- Steven A, Dickinson C, Pearson P. Practice-based interprofessional education: looking into the black box. J Interprof Care. 2007 Jun;21(3):251-64. PubMed PMID: 17487704.
- Robson M, Kitchen SS. Exploring physiotherapy students’ experiences of interprofessional collaboration in the clinical setting: a critical incident study. J Interprof Care. 2007 Feb;21(1):95-109. PubMed PMID:17365377.
- Copley JA, Allison HD, Hill AE, Moran MC, Tait JA, Day T. Making interprofessional education real: a university clinic model. Aust Health Rev. 2007 Aug;31(3):351-7. PubMed PMID: 17669056.
- Liedtka JM, Whitten E. Enhancing care delivery through cross disciplinary collaboration: a case study. J Healthc Manag. 1998 Mar-Apr;43(2):185-203; discussion 203-5. PubMed PMID: 10179019.
- Phelan AM, Barlow CA, Iversen S. Occasioning learning in the workplace: the case of interprofessional peer collaboration. J Interprof Care. 2006 Aug;20(4):415-24. PubMed PMID: 16905489.
Mental Health
- Kinnair DJ, Anderson ES, Thorpe LN. Development of interprofessional education in mental health practice: Adapting the Leicester Model. J Interprof Care. 2012 May;26(3):189-97. Epub 2012 Jan 17. PubMed PMID: 22250705.
- Priest HM, Roberts P, Dent H, Blincoe C, Lawton D, Armstrong C. Interprofessional education and working in mental health: in search of the evidence base. J Nurs Manag. 2008 May;16(4):474-85. PubMed PMID: 18405264.
- Craven MA, Bland R. Better practices in collaborative mental health care: an analysis of the evidence base. Can J Psychiatry. 2006 May;51(6 Suppl 1):7S-72S. Review. PubMed PMID: 16786824.
- Coleman MT, Roberts K, Wulff D, van Zyl R, Newton K. Interprofessionalambulatory primary care practice-based educational program. J Interprof Care. 2008 Jan;22(1):69-84. PubMed PMID: 18202987.
- Bradley P, Cooper S, Duncan F. A mixed-methods study of interprofessional learning of resuscitation skills. Med Educ. 2009 Sep;43(9):912-22. PubMed PMID: 19709016.
- McNair R, Brown R, Stone N, Sims J. Rural interprofessional education: promoting teamwork in primary health care education and practice. Aust J Rural Health. 2001 Dec;9 Suppl 1:S19-26. PubMed PMID: 11998271.
-
Interprofessional Education and Collaboration Matrix +
-
Rodgers, et al (2010), on behalf of the World Health Organization Study Group on Interprofessional Education and Collaborative Practice, conducted a global environmental scan of interprofessional education (IPE), they found that despite the existence of clearly recognized best practice evidence, IPE initiatives tended to be voluntary, were not founded upon specific learning objectives, lacked assessment and evaluation regarding there impact, and were not provided by instructors who were trained in facilitating IPE activities.
Hean et al. (2012), stress the need to anchor interprofessional initiatives in theory, and numerous systematic reviews have highlighted the need to design such initiatives based upon best practice evidence.
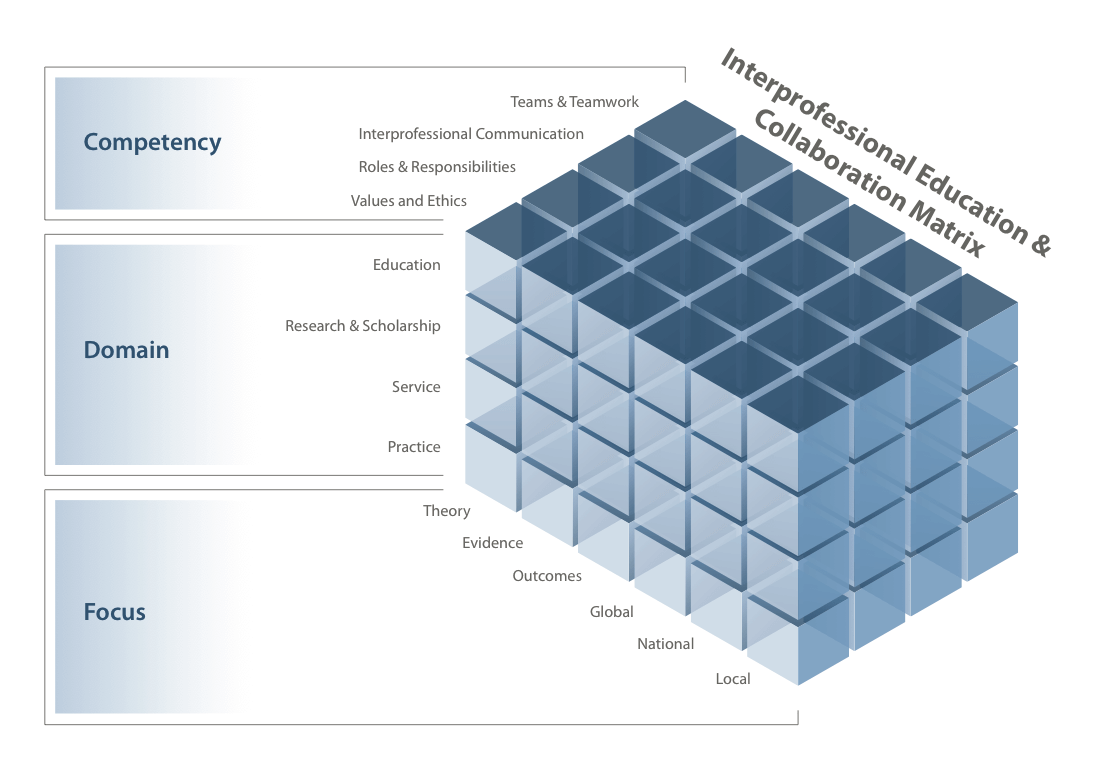
This matrix was developed to illustrate and draw attention to, the key components of interprofessional education and collaboration, and to assist in gathering and organizing, resources and evidence, for those interested in gaining an understanding of interprofessional education and collaboration. Each block of the matrix represents an intersection of a domain (e.g.education), competency (e.g. values and ethics) and focus (e.g. theory).
This design of this site attempts to complete each block within the matrix, reflecting the current theoretical perspectives, available evidence, and outcome measures, it also provides information on global, national, and ATSU interprofessional initiatives. This site is intended to be a resources for those in the process of developing or refining interprofessional initiatives.
-
Interprofessional Education Best Practice +
-
Rodgers et al (2010) describe the following five evidence-based best practices, drawn from the World Health Organization’s Framework for Action on Interprofessional Education and Collaborative Practice (WHO, 2010).
IPE should be:
- A mandatory component of every health professional’s education
- Offered based on explicit learning outcomes that are made clear to both staff and students
- Assessed with respect to what students were intended to learn
- Offered by trained facilitators who have received staff development in this area
- Evaluated for both process and outcomes
Supporting Literature
- Institute of Medicine (2001), Hoffman & Harnish (2007) and Ho, Jarvis-Selinger, Borduas, Frank, Hall, Handfield-Jones et al. (2008)
- Ramsden (2003), Freeth, Hammick, Reeves, Koppel, & Barr (2005), Norton (2009) and Thistlethwaite & Moran (2010)
- Freeth et al. (2005) and Biggs & Tang (2007)
- Hammick et al. (2007), Lindqvist et al. (2008) and Hammick et al. (2009)
- Barr et al. (2000), Hammick (2000), Freeth et al. (2002), Barr et al. (2005) and Reeves et al. (2008)
-
Courses +
-
Core Course: ASDOH IPE +
COURSE NAME: Dental Disciplines
MODULE NAME: Interprofessional Education Through the Lens of Oral Systemic Disease
MODULE NUMBER: 694
MODULE DESCRIPTION:This module consists of multiple sections that will begin during the fall of your D1 year and extend to the spring of your D2 year. The sections will include:- Interprofessional Education in Healthcare: this section will introduce students to the Interprofessional education in healthcare by exploring the concept and value of interprofessional education.
- Introduction to Collaborative Practice through Telehealth: this section introduces the concepts of telehealth (telemedicine and teledentistry) and will provide a basic understanding of how telehealth brings care to underserved populations utilizing traditional and new technologies. (D2 & D3)
- Communicating Universal Language in Health Care: this section is designed to teach students universal communication skills with patients and other healthcare providers.
Module Goals:
- Define and apply interprofessional education in the health care system.
- Apply the concept of interprofessional collaborative practice.
- Describe the process of team development and the role and practices of effective team.
- Describe current trends, technologies, appropriate uses of, and concerns with using telehealth (telemedicine and teledentistry) modalities
- Apply a foundation of theoretical knowledge that they will be able to transfer to their telehealth clinical rotation.
- Identify and define dental and medical auxiliaries and their roles on a dental and/or medical team
- Explain how to use and select the appropriate dental and medical codes based on a diagnosis
Elective Course: Interprofessional Cross-campus Collaborative Case +
The ICCC on the Missouri Campus involves a collaboration with Truman State University (TSU) health professions disciplines and the ATSU IPE office in Mesa. In 2014, the KCOM Curriculum Committee approved ICCC as an elective for KCOM students and 2016 the MOSDOH Curriculum Committee approved ICCC as an elective. Also, in 2016, a sixth discipline, Social and Cultural Sciences was added to the program. The semester-long CCC course allows students to work in teams to develop leadership skills and learn about, from and with other health professions disciplines. Student teams are provided a complex web-based case that they use to develop a patient/family-centered care plan that focuses on interprofessional teamwork, patient safety, and quality of care.
Over 80% of all students report that they would recommend ICCC to other students. One student commented, “I absolutely would recommend this program to another student. It was a wonderful learning experience.”
Course Description: Students participate in an orientation session where they are introduced to their multi-disciplinary team members and strategize how they will design their plan of care. New in 2016, two workshops were offered to students. Social work and hospice were presented by TSU professor, Rebecca Zimmer, MSW, LCSW and Carla Hustead, MSW, LCSW. The second workshop focused on presentation skills where students were given the opportunity rehearse, receive feedback and make amendments. As the culminating course activity, student teams present their plan of care using Google Slides to a panel of faculty members and community professionals. ICCC concludes with an evening of review and reflection for the students and faculty.
Elective Course: Interprofessional Health Partners +
Hours of Service to local elders provided by students – 2016: 405 hours and 2017: 372 hours
Former information visit the health partners site
“The interdisciplinary option (IPHC) within the House Calls program was created in 2002 in response to emerging national concerns related to improving healthcare and reducing medical errors,” said Janet Head, RN, MS, EdD, co-director, ATSU-KCOM AHEC and ATSU Aging Studies project director for the Kirksville campus.
Evolving from the Interprofessional House Calls elective, our current interprofessional home visiting program is an approved elective course that offers ATSU medical and dental students the opportunity to work with Truman State University students from five health disciplines. They work in interprofessional teams with community elders. In fall of 2015, IPHP was approved as an elective for MOSDOH students. Our main elective for the spring semester, IPHP allows students the opportunity to learn about other health disciplines, work with older adults, and enhance teamwork and communication skills.
Course Description: The course offers an orientation session that introduces key elements from the InterProfessional Education Collaborative (IPEC) core competencies, the Hartford Geriatric Interdisciplinary Team Training Curriculum (GITT), and TEAM STEPPS® a program designed to increase health care providers’ awareness of roles and responsibilities, communication skills, and ability to resolve conflict to enhance the quality of care and patient safety. Also during orientation, students become acquainted with the members of their team and are provided elder specific information. Review sessions are facilitated by faculty from ATSU and TSU. At each review session new screening tools are introduced and/or demonstrated; in addition, students report their findings and entertain questions and/or dialogue from other table team members.
Elective Course: Individual Cognitive Stimulation Therapy (iCST) +
A newly added KCOM elective, Individual Cognitive Stimulation Therapy was added to the elective catalog December 2016 with the first cohort of students beginning January 2017.
Individual CST evolved from the evidence-based group CST program developed in the United Kingdom at the University College of London. Through research, CST has been shown to improve the quality of life for those with mild to moderate dementia and at times improve cognition and language skills. Individual CST was designed for caregivers in the home as a way of engaging and interacting with the person diagnosed with dementia.
Students are introduced to the concept and key principles of iCST through a Zoom video conference with Saint Louis University. Students are placed in teams of two. Ten home visits are required for this course and students are required to create and develop a lesson plan for each visit according to the iCST guidelines and key principles. They document each visit, and complete reflective writing assignments. Three review sessions are conducted to allow students the opportunity to discuss challenges, report on their visits, and prepare materials for upcoming sessions. Assessment tools utilized for the program are introduced and students practice using the assessment tools on community volunteers. The final review session, includes a lecture on Dementia: Diagnosis and Treatment. Student evaluations are uniformly positive, and all participants have indicated that they would recommend this program to another student.
Interprofessional Education in Pre‐registration Courses +
A CAIPE Guide for Commissioners and Regulators of Education
Prepared by Hugh Barr and Helena Low, January 2012 © CAIPE 2012
Interprofessional Education in Pre-registration Courses
-
Collaborative Cases +
-
2017 Cross Campus Interprofessional Collaborative Case
2016 Cross Campus Interprofessional Collaborative Case
2015 Cross Campus Interprofessional Collaborative Case
2014 Cross Campus Interprofessional Collaborative Case
2013 Cross Campus Interprofessional Collaborative Case
2012 Cross Campus Interprofessional Collaborative Case
-
IPE Grants +
-
CDC/APTR Grant - Population Health Case Studies: Impacting Health Through Evidence-Based Community and Clinical Interventions
Expanding Dental Workforce Training with Collaborative, Team-Based Care, Targeting FQHC/ Underserved Populations
MAHEC: A Statewide Network for Interprofessional Healthcare Workforce Development and Practice Transformation in Rural and Underserved Missouri
-
Core Competencies +
-
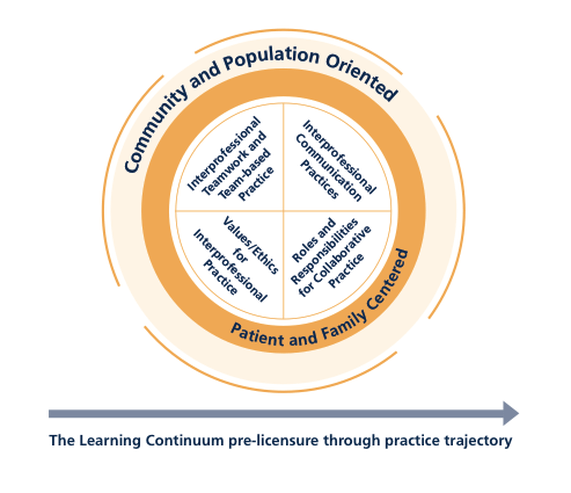
1: Values/Ethics for Interprofessional Practice+
General Competency Statement-VE.
Work with individuals of other professions to maintain a climate of mutual respect and shared values.Specific Values/Ethics Competencies:
VE1. Place the interests of patients and populations at the center of interprofessional health care delivery and population health programs and policies, with the goal of promoting health and health equity across the life span.
VE2. Respect the dignity and privacy of patients while maintaining confidentiality in the delivery of team-based care.
VE3. Embrace the cultural diversity and individual differences that characterize patients, populations, and the health team.
VE4. Respect the unique cultures, values, roles/responsibilities, and expertise of other health professions and the impact these factors can have on health outcomes.
VE5. Work in cooperation with those who receive care, those who provide care, and others who contribute to or support the delivery of prevention and health services and programs.
VE6. Develop a trusting relationship with patients, families, and other team members (CIHC, 2010).
VE7. Demonstrate high standards of ethical conduct and quality of care in one’s contributions to team-based care.
VE8. Manage ethical dilemmas specific to interprofessional patient/ population centered care situations.
VE9. Act with honesty and integrity in relationships with patients, families, and other team members.
VE10. Maintain competence in one’s own profession appropriate to scope of practice.© 2016 IPEC®.
2: Roles/Responsibilities+
General Competency Statement-RR.
Use the knowledge of one’s own role and those of other professions to appropriately assess and address the healthcare needs of patients and to promote and advance the health of populations.Specific Roles/Responsibilities Competencies:
RR1. Communicate one’s roles and responsibilities clearly to patients, families, community members, and other professionals.
RR2. Recognize one’s limitations in skills, knowledge, and abilities.
RR3. Engage diverse professionals who complement one’s own professional expertise, as well as associated resources, to develop strategies to meet specific health and healthcare needs of patients and populations.
RR4. Explain the roles and responsibilities of other care providers and how the team works together to provide care, promote health, and prevent disease.
RR5. Use the full scope of knowledge, skills, and abilities of professionals from health and other fields to provide care that is safe, timely, efficient, effective, and equitable.
RR6. Communicate with team members to clarify each member’s responsibility in executing components of a treatment plan or public health intervention.
RR7. Forge interdependent relationships with other professions within and outside of the health system to improve care and advance learning.
RR8. Engage in continuous professional and interprofessional development to enhance team performance and collaboration.
RR9. Use unique and complementary abilities of all members of the team to optimize health and patient care.© 2016 IPEC®.
3: Interprofessional Communication+
General Competency Statement-CC.
Communicate with patients, families, communities, and professionals in health and other fields in a responsive and responsible manner that supports a team approach to the promotion and maintenance of health and the prevention and treatment of disease.Specific Interprofessional Communication Competencies:
CC1. Choose effective communication tools and techniques, including information systems and communication technologies, to facilitate discussions and interactions that enhance team function.
CC2. Communicate information with patients, families, community members, and health team members in a form that is understandable, avoiding discipline-specific terminology when possible.
CC3. Express one’s knowledge and opinions to team members involved in patient care and population health improvement with confidence, clarity, and respect, working to ensure common understanding of information, treatment, care decisions, and population health programs and policies.
CC4. Listen actively, and encourage ideas and opinions of other team members.
CC5. Give timely, sensitive, instructive feedback to others about their performance on the team, responding respectfully as a team member to feedback from others.
CC6. Use respectful language appropriate for a given difficult situation, crucial conversation, or interprofessional conflict.
CC7. Recognize how one’s own uniqueness, including experience level, expertise, culture, power, and hierarchy within the health team, contributes to effective communication, conflict resolution, and positive interprofessional working relationships (University of Toronto, 2008).
CC8. Communicate consistently the importance of teamwork in patient- centered care and population health programs and policies.© 2016 IPEC®.
4: Teams and Teamwork+
General Competency Statement-TT.
Apply relationship-building values and the principles of team dynamics to perform effectively in different team roles to plan, deliver, and evaluate patient/population-centered care and population health programs and policies that are safe, timely, efficient, effective, and equitable.Specific Team and Teamwork Competencies:
TT1. Describe the process of team development and the roles and practices of effective teams.
TT2. Develop consensus on the ethical principles to guide all aspects of team work.
TT3. Engage health and other professionals in shared patient-centered and population focused problem-solving.
TT4. Integrate the knowledge and experience of health and other professions to inform health and care decisions, while respecting patient and community values and priorities/ preferences for care.
TT5. Apply leadership practices that support collaborative practice and team effectiveness.
TT6. Engage self and others to constructively manage disagreements about values, roles, goals, and actions that arise among health and other professionals and with patients, families and community members.
TT7. Share accountability with other professions, patients, and communities for outcomes relevant to prevention and health care.
TT8. Reflect on individual and team performance for individual, as well as team, performance improvement.
TT9. Use process improvement strategies to increase the effectiveness of interprofessional teamwork and team-based services, programs, and policies.
TT10. Use available evidence to inform effective teamwork and team-based practices.
TT11. Perform effectively on teams and in different team roles in a variety of settings.© 2016 IPEC®.
-
Global and National Initiatives +
-
National Activities within the USA
- American Interprofessional Health Collaborative (AIHC) - This organization is a great source for information on interprofessional activities within US Colleges and Universities. AIHC is aligned with the National Center for Interprofessional Practice and Education.
- National Center for Interprofessional Practice and Education - The National Center is charged to provide the leadership, evidence and resources needed to guide the nation on interprofessional education and collaborative practice.In that pursuit, we aim to challenge tradition and create a deeply connected, integrated learning system that will transform education and care together
- National Academies of Practice (NAP) - Distinguished professionals advancing interprofessional healthcare by fostering collaboration and advocating policies in the best interest of individuals and communities. NAP is a collaboration between 14 professional academies.
Global Initiatives
International Interprofessional Organizations
There are many excellent resources available through international organizations dedicated to promoting interprofessional education and collaboration.The World Coordinating Committee for Interprofessional Education and Collaborative Practice - All Together Better Health
- AFRIPEN - The Sub-Saharan African Interprofessional Education Network
- AIHC - The American Interprofessional Health Collaborative (USA)
- AIPPEN - The Australasian Interprofessional Practice and Education Network (Australia and New Zealand)
- CAIPE - The (UK) Centre for the Advancement of Interprofessional Education
- CIHC - The Canadian Interprofessional Health Collaborative
- EIPEN - The European Interprofessional Practice and Education Network
- JAIPE - The Japan Association for Interprofessional Education
- JIPWEN - The Japan Interprofessional Working and Education Network
- NIPNET - The Nordic Interprofessional Network (Nordic countries in Europe)
Useful Resources
- Interprofessional Collaborative Practice and Learning Environments
- eLearning: Interprofessional and inter-agency collaboration (IPIAC) - This British site provides free e-learning resources including, audio, video and interactive technology. The aim is to help share resources that can assist in exploring the nature of interprofessional and inter-agency collaboration and in improving collaborative practice.
-
Key Documents +
-
 WHO Framework for Action on Interprofessional Education and Collaborative Practice
WHO Framework for Action on Interprofessional Education and Collaborative Practice
 Interprofessional Education in Pre-Registration Courses: A CAIPE Guide for Commissioners and Regulators of Education
Interprofessional Education in Pre-Registration Courses: A CAIPE Guide for Commissioners and Regulators of Education
 Core Competencies for Interprofessional Collaborative Practice: 2016 Update
Core Competencies for Interprofessional Collaborative Practice: 2016 Update
 Interprofessional Education Collaborative (IPEC)
Interprofessional Education Collaborative (IPEC)
Core Competencies for Interprofessional Collaborative Practice
-