The human curriculum: ATSU’s standardized patient programs prepare students for real-life care
Posted: April 15, 2026
Every healthcare professional remembers the first time they sat face to face with a patient. They remember the nerves, the uncertainty, and the responsibility. At ATSU, students experience that moment earlier than most, through standardized patient (SP) programs designed to help students build confidence and enhance skills before they ever step into real-world practice.
Encounter dialogue
Student: “Hello, I’m Student Doctor Peyton Grant. What brings you in today?”
Patient: “I’ve been having some pain in my shoulder.”
Student: “Can you tell me exactly where your pain is located?”
Patient: “It’s my right shoulder. I fell on it a few days ago, and it’s not getting better.”
Student: “Can you describe your pain?”
Patient: “It’s a sharp pain when I move it, but a constant, dull ache when I’m resting.”
Student: “On a scale of 1-10, with 1 being very little pain and 10 being the most pain you’ve ever experienced, how would you rate your pain?”
Patient: “Right now, maybe a 4. But when I try to lift my arm, it’s a 7 or 8.”
Student: “What caused you to fall?”
Patient: “I was walking my dog. She chased a squirrel, and I tripped over the leash and landed on
my right side …”

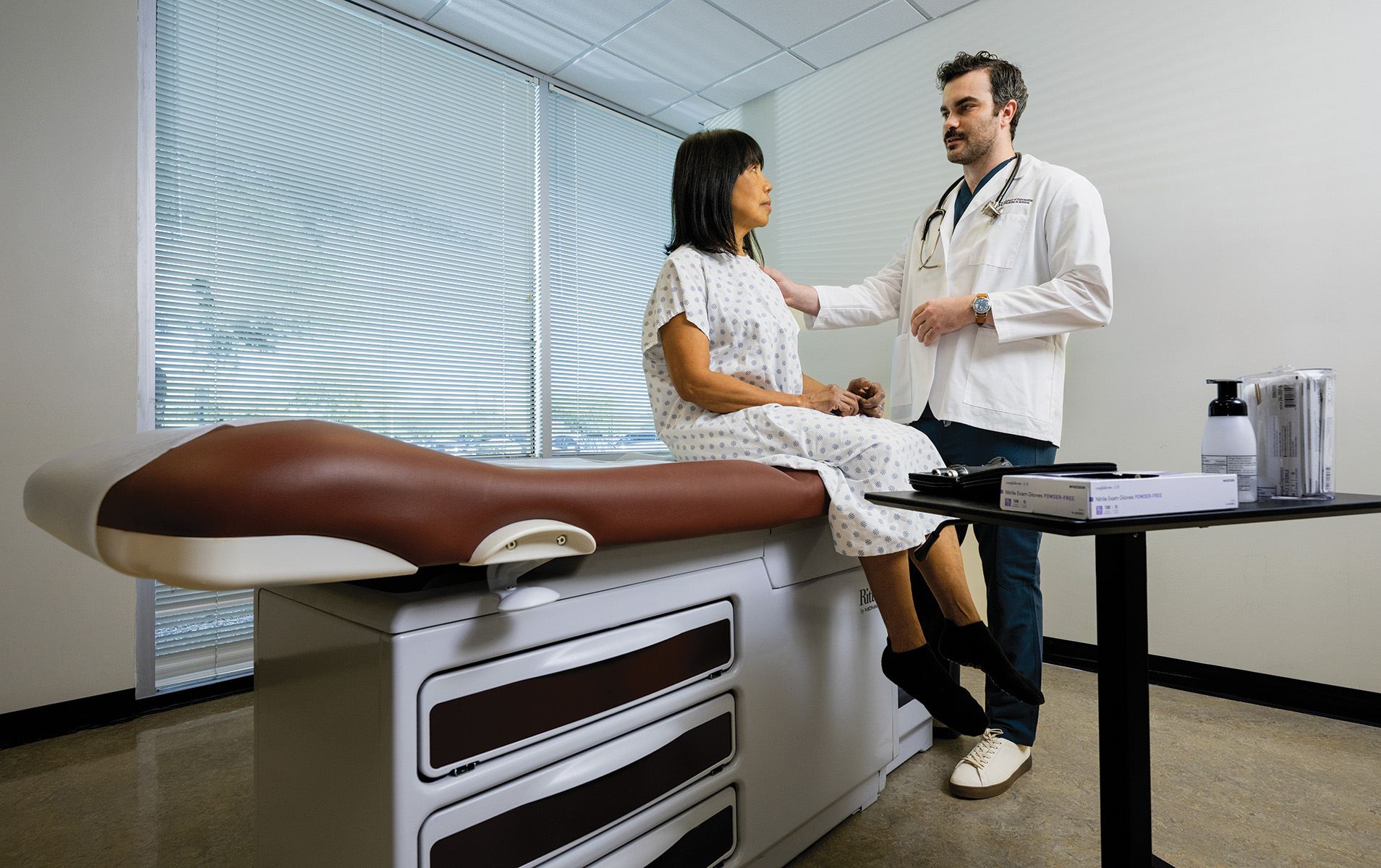
An SP encounter looks like a routine clinical visit: a patient, a student provider, and a conversation about symptoms and concerns. But behind the scenes, every word and response is carefully designed to help ATSU students learn the practice of quality patient care. Across campuses, SP visits turn simulated educational encounters into powerful learning experiences.
SPs are real-life people who are taught to portray patients in realistic and repeatable ways. They are given character names, personalities, and scripts to follow with specific histories, conditions, and symptoms. SP encounters allow students to apply their knowledge and skills in a safe, simulated environment without jeopardizing real patients. These encounters also allow students to reflect, build confidence, and improve their interactions with patients, ultimately preparing them to provide high-quality healthcare on day one.
SPs have been part of medical education for decades, with ATSU’s first standardized patient program beginning at Kirksville College of Osteopathic Medicine (ATSU-KCOM) more than 25 years ago. Today, SP programs have spread across ATSU campuses for many academic programs, including Osteopathic Medicine (DO), Physician Assistant Studies (PA), Physical Therapy (PT), Occupational Therapy (OT), Dental Medicine, Audiology, and Speech-Language Pathology (SLP).
ATSU’s SP encounters are set up in individual patient rooms designed like those of a real clinic. Nearby, a control room equipped with an audio-visual system allows staff members to monitor encounters and record interactions between students and patients. Once encounters are complete, students receive feedback and watch their recordings to see what they did well and what aspects could be improved.
The SP program based in Kirksville, Missouri, is housed in the Byron & Helena Greenberg Performance Assessment Center (PAC), designed specifically for SP encounters. Lisa Archer, BSN, RN, CHSE, director of simulation & performance assessment, ATSU-KCOM, oversees the Missouri SP program. She and her team work year-round to ensure SPs are well prepared to portray real patients and to ensure students gain valuable experience and quality feedback.
Since joining ATSU in 2014, Archer has led the expansion of all Missouri-based simulated learning experiences, including SP encounters. Not only do medical students at ATSU-KCOM complete encounters, but so do dental students from ATSU’s Missouri School of Dentistry & Oral Health (ATSU-MOSDOH), as well as nursing students from Truman State University and local family medicine residents. Bringing together students from different disciplines allows opportunities for interprofessional education (IPE), including mental health SP encounters for DO and nursing students. Additionally, the SP program includes Spanish-speaking SPs for the ATSU-KCOM Medical Spanish elective course, where SP encounters are conducted entirely in Spanish.
“The school has long invested in the program to make sure it has all the resources needed to develop and grow it,” says ATSU-KCOM Dean Margaret Wilson, DO, ’82. “This includes hiring dedicated SPs who are well prepared to portray real-life scenarios and able to critically evaluate student performance.”
Kathy Schroeder has served as the Missouri SP educator since 2015. Prior to this role, she was an SP for eight years, which gave her firsthand experience with the SP learning curve. Drawing on her expertise, she has helped build a team consisting of 57 SPs, along with nine Medical Spanish SPs. Additionally, Marianne Romprey serves as the SP support specialist, scheduling encounters and running the software, and Rob Long serves as the simulation specialist, ensuring the technology functions smoothly.

Additionally, the Missouri SP team includes 10 SP mentors, who are highly experienced SPs. These mentors are paired with new SPs to help them learn their role and support them throughout the orientation process, ensuring a consistent level of quality among team members.
“From the beginning, Dr. Wilson has believed so strongly in this program that we’ve pulled out all the stops, and this is what we pour into our students’ education,” Archer says.
The approach to quality education and well-prepared graduates extends throughout ATSU to its Mesa, Arizona, and Santa Maria, California, campuses. In 2007, ATSU’s School of Osteopathic Medicine in Arizona (ATSU-SOMA) officially began its SP program with the graduating class of 2011. In 2019, the Clinical Performance Center (CPC) opened on the Arizona campus, providing a dedicated home for SP encounters, skills labs, and classroom instruction.
“SPs are foundational to how we train osteopathic physicians at ATSU-SOMA,” says Christina Weaver, DO, ’14, assistant dean, innovation & clinical curricular integration. “From the very first week of medical school, students develop communication skills, empathy, and clinical presence through meaningful interactions with SPs, followed by thoughtful feedback that supports their growth. While technology plays an important role in simulation, SPs offer the highest level of realism, mirroring the complexity, nuance, and humanity of real clinical encounters.”
In addition to ATSU-SOMA, SPs are used by several programs at ATSU’s Arizona School of Health Sciences (ATSU-ASHS), including PA, PT, OT, SLP, and Audiology. ATSU’s Arizona School of Dentistry & Oral Health uses SPs for interviewing applicants to the School and for students to practice patient-centered interviewing.
“Within the CPC, students engage in realistic patient encounters in fully equipped clinical examination rooms, allowing them to apply clinical knowledge in an authentic environment,” says Brittney Hulsey, DMSc, ’22, MSPAS, ’15, MS, PA-C, program director and associate professor, physician assistant studies. “At the conclusion of each clinical medicine course, students are formally assessed through observed encounters with SPs, with performance evaluated by faculty proctors.”
With the variety of programs on the Arizona campus, the CPC provides IPE opportunities using SPs. For example, the OT program collaborates with the SLP program for its Basic Patient Care Skills course where OT and SLP students conduct an intake evaluation with SPs to practice their evaluation skills. Also, DO and dental students collaborate on SP-based activities to learn from each other and improve patient outcomes.
Although programs incorporate SPs differently into their curricula, the purpose is the same: enhance student learning to produce well-rounded, high-quality healthcare providers. Faculty across disciplines echo the benefits of the CPC’s impact on student learning and assessment.
“The use of the center, along with the participation of multiple SPs, has been invaluable, and we have received outstanding support from the CPC staff throughout each experience,” says María A. Centeno-Vázquez, PhD, CCC-SLP, BCS-S, chair, program director, and associate professor, speech-language pathology. “Our faculty are actively involved by directly observing students during these encounters and facilitating structured debriefing sessions afterward.”

The Arizona campus employs about 70 SPs, all educated and coordinated through the CPC. The CPC is led by Lorena Navarro, BSN, MSHS, CHSE, who joined ATSU in January 2025. Navarro works closely with four other team members: Lindsey Bowen, CPC operations coordinator; Josie Penrod, CPC SP coordinator; David Godziela, CPC simulation & technology specialist; and Moira Caswell, CPC simulation coordinator & technologist.
“What I enjoy most about our SP program at the CPC are the people – the team, the SPs, and the learners they help shape,” says Navarro. “Our SPs bring an extraordinary level of authenticity, professionalism, and commitment to healthcare education.”
Bowen and Penrod, both with years of experience as SPs themselves, lead much of the SP instruction. They both joined the team in 2019 after being SPs for seven years. Together, they ensure SPs are taught to portray patients authentically and provide meaningful, patient-centered feedback. Godziela, who joined the team in October 2025, ensures each encounter runs smoothly and students and faculty can focus on learning.
“I love being able to build and train an amazing team of SPs who know how to portray a patient in so many different aspects,” says Bowen. “They are trained to help students be prepared to go out into the real world and not only how to interact with their patients on a doctor level but also on a level that connects them with their patients compassionately and empathetically.”
Caswell focuses on creating high-fidelity environments, ensuring the environment looks and feels real. Like Bowen and Penrod, Caswell also has SP experience. Before joining ATSU in November 2025, she worked as an SP for two years at other local institutions. She says working in the CPC is the one place where her “quirky” resume makes sense.
“I love using my theater background to set the stage and my clinical background to ensure it’s medically accurate. There is a thrill in creating a high-fidelity environment, whether through moulage or tech, that helps a student suspend disbelief and learn how to save a life,” Caswell says. “On a personal level, I love the reputation of this specific program. When I was working as an SP at other institutions, actors always spoke of ATSU as the ‘gold standard.’ Now that I am here as a tech, I see why. The SPs are incredibly dedicated, and it is a privilege to support a team that strives for that level of excellence.”
The number of SP encounters students complete varies by academic program, and several programs require students to demonstrate clinical competencies to graduate. DO students complete between 38-45 encounters in their programs, while PA students participate in about 15. Dental, SLP, OT, and PT students usually complete fewer than 10 SP encounters across their programs, and the Audiology program uses SPs 3-4 times a year. Additionally, both campuses follow best practices established by the Association of Standardized Patient Educators to ensure the growth, integrity, and safe application of SP encounters.
On the California campus, ATSU’s College for Healthy Communities is establishing its SP program for PA students. Currently, students are playing the role of SPs, acting as both clinician and patient and alternating roles across two clinical cases of equivalent complexity. To maintain clinical unpredictability and preserve the assessment’s integrity, peer pairs are randomized, ensuring students cannot anticipate their partner’s presentation or communication style. Jacqualine Dancy, MPAS, PA-C, associate professor, says moving forward, their program will adopt a hybrid model, integrating community members and peer SPs to provide a multifaceted, longitudinal learning experience preparing students for the transition from classroom to clinic.
“While community SPs provide a higher degree of realism, the peer-led model offers distinct pedagogical advantages,” says Dancy. “The presence of a known peer provides a degree of psychological safety, allowing students to refine their clinical skills in a supportive, low-stakes environment while gaining a dual perspective that enhances both medical acumen and professional empathy.”
The SP family
At ATSU, SPs are not merely paid actors; they are community members of all backgrounds and professions who are invested in their local students’ education. They spend hours studying and preparing to become valuable pieces of the educational experience.
“I look at being an SP as something special and valuable that I can contribute to this world where healthcare is a global concern,” says Jessie Cragg, a Missouri campus SP of 14 years and an SP mentor. “I think of my SP job as helping student doctors learn to help people everywhere.”
Greg Chugg has been an Arizona campus SP for about 18 years. He always had an affinity for the medical field and joined the program after an early retirement. One of his favorite aspects of the SP program is watching students grow and contributing to their education.
“When they first come in, they’re totally lost,” he says. “But within a few weeks, they really catch on. It’s exciting to see how quickly they progress.”
In addition to seeing the students grow, Chugg has also seen the SP program grow. He started as one of the original Arizona campus SPs. He also worked full time as a simulation technician for many years. Today, he continues serving as an SP, working on a part-time basis.


For many SPs, longevity in the role is tied not only to its flexibility but also its impact. Heidi Buckmister, who’s been an SP on the Arizona campus since 2017, says being an SP allows her to work and still prioritize her family. She also says being an SP has opened her eyes to patient needs across the country.
“Through this program, I was able to learn about food deserts and barriers to access to healthcare,” Buckmister says. “I didn’t know anything about that until I worked in this program and saw the real everyday struggles people go through. It’s been very humbling.”
Taking on the role of an SP is eye-opening for many reasons. Tammy Whitworth, a Missouri SP mentor, was a registered nurse who decided to change careers after the pandemic. She wanted a career that would be flexible and still allow her to make a difference.
“Having worked with hundreds of providers over a 36-year career, I know what good bedside manner looks like,” she says. “I had to take off my nurse hat completely and put myself in the shoes of a patient.”
Eric Ensign, also a Missouri SP mentor, has gained a greater understanding of medical issues as well as the process students go through to provide appropriate care. Because of this knowledge, he says he will never experience his personal doctor appointments the same way he did before becoming an SP.
“It’s impossible for me to sit in an exam room and not evaluate the process of care,” he says. “At the same time, I have a greater appreciation for what the nurses and doctors have to accomplish in the relatively short time they are interacting with me.”
In SP encounters, students have a checklist of questions to ask their patient, along with time limits. Similarly, SPs have a checklist of structured feedback to provide to students after their encounter, along with written feedback describing observed behaviors paired with suggestions for improvement. One of the many important aspects of educating SPs for their roles is how they must evaluate students according to the standards, not their personal preferences.
“What has surprised me is how these students’ personalities really come forth in the encounters,” Cragg says. “The students all have the same guidelines, and the SPs all have the same ‘script,’ yet every encounter is a fresh new experience!”
Across campuses, SPs echo a sense of pride in being part of the University and part of a process to enhance the quality of future healthcare providers. Missouri SP mentor Peggy Gerhold says while it may appear SPs are just sitting on the exam table playing their role with a look of pain on their face, inside, they are cheering on each student.
“They treat you like a real patient, and they take it seriously,” says Mia Mickley, an Arizona SP since 2014. “They are so open to feedback and are very invested in their future.”
“I really enjoy my interactions with everyone, whether it’s other SPs, the facilitators, or the students,” says Kathy Walker, an Arizona SP. “It feels like a family, it always has since day one.”
The SP teams on each campus have naturally formed their own “family” units. Besides working together, they support and celebrate each other, and even spend time together outside of their SP roles.
“These are people who love ATSU,” Archer says. “They love being part of something that has such a strong purpose – educating the future physicians of our community and our world.”
To learn what SPs have to say about their roles and preparing ATSU students for real patient care, visit atsu.edu/sp-patients
The future physicians
Libbi Kleitz, a second-year ATSU-KCOM student, felt a mix of excitement and nervousness before her first SP encounter. Much like every “first” of medical school, she felt encouraged by the faculty and peers around her who assured her this would be a beneficial learning experience. Once her encounter began, she says her nerves seemed to calm and her newly formed muscle memory took over.
“I felt like I could connect with my patient on a personal level while simultaneously scribbling through COPMAPS, our mnemonic for history taking,” she says. “There is a certain empowerment that comes with feeling yourself grow in real time; that is what SP encounters are all about.”
ATSU-KCOM’s method for ensuring a comprehensive patient assessment is COPMAPS, a mnemonic used by students for taking a patient’s history. It follows the order of complaint (quality, location, severity, quantity), onset (how, when), progression, mitigating factors, associated symptoms, previous occurrence/pertinent other, and summarize. Students are encouraged to write this mnemonic down the side of their paper before they go into patient rooms to take notes.
“There are real patients who are tight-lipped, stoic, and shy, and if the doctor doesn’t ask the question, they won’t divulge that information,” Archer says. “We have to train our students to get a good history with all the data points they need, and COPMAPS helps us accomplish that.”



For ATSU-SOMA and ATSU-ASHS PA students, their mnemonic for patient assessment is OLDCARTS. This memory aid follows the order of onset, location, duration, characteristics, aggravating/alleviating factors, radiation, timing, and severity.
First-year ATSU-SOMA student Tim McGinley says working with SPs has been an invaluable part of his education. In addition to having the opportunity to learn from mistakes in a controlled environment, he believes the SP experience provides important self-awareness.
“The best part about working with SPs is seeing where I’m strongest and where I can improve,” he says. “I really value the interpersonal aspect of medicine, and being able to work with SPs is a real honor.”
Marshall Brace, an ATSU-KCOM medical education fellow, recalls the moment where all aspects of an SP encounter fell into place for him. He was performing a neurological examination on his SP and asked her to make a face. When she did, only part of her face moved. At first, he thought she misheard him, and he repeated the instruction, observing the same result.
“It was then it finally clicked and I realized that I was observing an abnormal result, jotting down in my notes ‘Right CN VII out,’” he says. “That was a great moment because we are so used to seeing the normal results of exams that being able to observe the abnormal findings gives a sort of ‘aha’ moment.”
For Noah Everson, a first-year ATSU-KCOM student, a similar moment shifted his mindset. In one of his SP encounters, the SP responded emotionally to a question, and instead of moving on to the next item in the checklist, he paused and acknowledged what the SP was feeling.
“I stopped thinking about points and objectives and focused on the patient in front of me,” Everson says. “The conversation became more natural, the patient opened up, and the encounter felt far more meaningful.”
Over time through multiple SP encounters, students learn to incorporate their mnemonic more smoothly into their patient interviews, and they find their own rhythm and flow. History taking becomes second nature, and each encounter becomes more of a conversation rather than a mere checklist.
“These encounters are showing me how important trust and consistency are over time,” says second-year ATSU-MOSDOH student Thomas Beddard. “They have also helped me learn how to calm patient anxiety, which can make a big difference in a patient’s willingness to accept treatment and come back in the future to maintain their oral health.”

Not only do students benefit from the repeated exposure to SPs and the variety of cases, but they also benefit from their feedback. Peyton Grant, an ATSU-KCOM medical education fellow, says after reading feedback from the SPs, she was reassured she was becoming the thoughtful and compassionate physician she hopes to be one day.
“I am confident that these experiences have equipped me to enter clinical rotations and subsequent patient care settings with greater confidence, compassion, and resilience,” she says.
Fourth-year ATSU-KCOM student Kathryn Carey says the feedback from SPs has significantly influenced how she communicates with her patients during clinical rotations, particularly in developing more professional and intentional language.
“During my first year, my friends and I frequently used the phrase ‘a little’ in casual conversation, and I did not initially realize I brought this into an SP encounter when I said, ‘I see you’re having a little chest pain,’” Carey says. “The feedback helped me understand that minimizing language like this can feel dismissive or demeaning to patients, even when that is not the intent.”
Carey also says SPs provided feedback about using too much medical jargon when explaining diagnoses or plans. This kind of feedback reinforces the importance of identifying health literacy and ensuring patients truly understand their condition so they can participate in their own care.
“The honesty of SPs makes this feedback especially valuable, as they often share perspectives that real patients may not feel comfortable expressing directly, allowing for reflection and the opportunity to meaningfully improve patient care,” she says.
Students recognize SPs are critical to their success as they transition from classroom to clinic. Katie Wilson, a second-year ATSU-KCOM student, says she saw this in action during a summer shadowing experience where she used COPMAPS while also tailoring her questions to fit the patient’s chief complaint.
“The physician I worked under was impressed with my abilities to do patient interviews, especially as an incoming second-year student, and allowed me to see most of their patients first, then give a report,” Wilson says.
“Practice makes perfect, and SP encounters start that practice early.”
-Ellie Cumpton, ATSU-KCOM medical education fellow
Not only do students appreciate the roles SPs play, but they also acknowledge how well they perform those roles. The variety of symptoms they present and the range and intensity of emotions they convey, including conversations on difficult topics, all contribute to the realism of these encounters.
“Our SPs are very clinically aligned with real patients, especially when it comes to communicating pain,” says first-year ATSU-SOMA student Jennifer Lanza. “I really feel like we’re in our rotations or working as an attending physician. It gives us that real-life feeling of being a doctor.”
Learn more about what ATSU students have to say about their experiences with standardized patients by visiting atsu.edu/sp-students
Lessons that last
Matt Burnett, DO, ’25, a resident physician at Trinity Health Ann Arbor, recalls the nerves and stress of participating in SP encounters as an ATSU-KCOM student. He remembers feeling the pressure of balancing multiple demands and the uncertainty each encounter brings. He also remembers feeling the evaluations were subjective to some degree.
“My counter to that now is that every real patient encounter is subjective, shaped by the patient’s beliefs, impressions, and emotions at the time,” Dr. Burnett says. “SP encounters teach students that how they behave, present themselves, and communicate always leaves an impression.”
Dr. Burnett believes students get out what they put into their encounters. When students approach their encounters with a positive attitude, it almost always benefits them in the long run. Furthermore, he says ATSU-KCOM’s curriculum is very intentional in how it progressively increases the level and amount of responsibility students take on before clinical rotations.
“SP encounters emphasized patient connection, building rapport, listening, introducing yourself and your role, performing a thorough physical examination, and communicating clearly,” Dr. Burnett says. “These fundamentals remain the foundation of every patient interaction I have today, and they now feel natural and reflexive.”
Michael Megafu, DO, MPH, ’24, an orthopedic surgery resident at the University of Connecticut, says he was fortunate to have many early patient experiences at ATSU-KCOM, including SP encounters, to enhance his skillset. Even in the midst of a busy day, he remembers to take time to speak with his patients, and not just about their pathology.
“I still rely on interpersonal skills and the ability to connect with patients, a soft skill I believe offers a valuable return on investment when used correctly,” Dr. Megafu says. “Patients appreciate a knowledgeable physician, but they are likely to continue with a doctor who actually listens to them, rather than one who has all the answers but is in a rush to see the next patient.”
Dr. Megafu says the volume and variety of encounters shouldn’t be taken for granted, even though they may be time consuming to prepare for and complete. He advises diligently working on assimilating all the information the patient provides to make a succinct, but thorough, summary of the patient’s presentation. By doing so, students will be able to arrive at a diagnosis quickly and manage their patients efficiently.
“I appreciate all the SPs who have taken the time to be a help and an asset to our education,” Dr. Megafu says. “Without them, we will greatly miss out on the importance of communication and will not be the quality student doctors and doctors that have been evident throughout the different clinical sites.”

To view behind-the-scenes footage of ATSU’s SP encounters, visit atsu.edu/sp-bts
Interested in becoming an SP?
Opportunities are available at all of ATSU’s campuses. Please contact the following for more information:
Kirksville, Missouri: Lisa Archer at larcher@atsu.edu
Mesa, Arizona: Lorena Navarro at lorenanavarro@atsu.edu
Santa Maria, California: Jacqualine Dancy at jacqualinedancy@atsu.edu