 |
*Escherichia coli (facultative)
Streptococcus spp. (microaerophilic) *Bacteroides fragilis (anaerobic) Clostridium spp. (anaerobic) Eubacterium spp. (anaerobic) Fusobacterium spp. (anaerobic) |
ID 821-824, 858-872
|
|
|
|
ETIOLOGICAL AGENTS:
Any organisms inhabiting the gastro-intestinal tract.
Most infections are polymicrobic and consist of both aerobes and anaerobes
with the anaerobes predominating. The most commonly-isolated species are:
 |
*Escherichia coli (facultative)
Streptococcus spp. (microaerophilic) *Bacteroides fragilis (anaerobic) Clostridium spp. (anaerobic) Eubacterium spp. (anaerobic) Fusobacterium spp. (anaerobic) |
OVERVIEW:
The healthy gastro-intestinal tract contains more than 100 species of bacteria, a limited number of viruses, and perhaps a few species of fungi and parasites. Various local and systemic, specific and non-specific immune mechanisms prevent the spread of these organisms to extra-intestinal sites. However, occasionally there are conditions which arise which compromise the intestinal immune mechanisms and allow tissue invasion by normal and abnormal intestinal flora.
These conditions include:
Antibiotic therapy
Neoplasm
Trauma
Cholecystitis
Obstruction
Ulceration
Diabetes mellitus
Pylephlebitis
Diverticula formation
Rubeola
An abscess, a localized collection of pus in a cavity formed by the disintegration of tissues, is the major manifestation of compromization of the gastrointestinal mucosa.
What differentiates the gastrointestinal abscess
from most other abscesses is the predominance of anaerobic bacteria within
the abscess. The significance of this lies in the unique characteristics
of anaerobes: relative antibiotic insensitivity, a capsule that is both
antiphagocytic and promotes abscess formation, a repertoire of enzymes
which promote virulence.
|
|
|||||
| Enzymes | B. fragilis
|
B. melaninogenicus
|
B. bivius | Bacteroides,
Other Sp. |
Fusobacterium Sp. |
| Hyaluronidase | X | ||||
| Collagenase | X | X | X | ||
| Condroitin sulfatase | X | ||||
| Fibrinolysin | X | X | |||
| Neurominidase | X | X | X | X | |
| Heparinase | X | ||||
| DNase | X | X | X | X | |
| IgM protease | X | ||||
| IgG protease | X | ||||
| IgA protease | X | ||||
| Superoxide | X | X | X | ||
| b-lactamase | X | X | X | X | X |
PATHOGENESIS:
The pathogenesis of infection with nonspore-forming anaerobes occurs in settings of reduced oxygen tension and oxidation-reduction potential in tissues that are normally well oxygenated and resistant to invasion by anaerobes. This may stem from an impaired blood supply, necrosis of tissue or growth of facultative bacteria. These conditions may be associated with vascular disease, trauma, surgery, presence of foreign bodies, malignancy, radiation therapy, injection of vasoconstrictive agents, shock, cold or edema. In these settings not only is an appropriate anaerobic environment obtained but other local host defenses are also impaired, thereby enabling these opportunists to initiate growth. Blood products (e.g., hemin, Fe3+, fibrin) produce an adjuvant effect and reduce the size of the inoculum required to produce infection.
In these settings, anaerobic bacteria initiate infection
by direct extension from membrane or cutaneous surfaces into normally sterile
adjacent tissue. Once bacteria are introduced into the affected site, the
production of toxins, enzymes and other virulence factors is significant.
The net result is localized tissue destruction and inflammation. Often
there are edema, hemorrhage, necrosis, thrombosis and hyperplasia of lymphoid
follicles. In protracted disease there is tissue granulation and nodular
aggregates of lymphoid cells. This may lead to perforation, spillage of
intestinal contents into the peritoneal cavity and general peritonitis.
CLINICAL SYMPTOMS:
Peritonitis. The mode of onset (acute vs. chronic) varies according to the precipitating cause.pical findings are pain, abdominal distention, absence of abdominal respiratory movement, diffuse muscle spasm, tenderness and rebound tenderness, decreased or absent perstalisis, rigidity of the abdominal wall, tenderness on rectal or vaginal examination, fever and leukocytosis.
Appendicitis and Diverticulitis. Abdominal pain, signs of peritoneal irritation, fever and leukocytosis are the major clinical findings in appendicitis and diverticulitis. There are, however, important differences in the patterns of these manifestations. Pain is the principal and often the only symptom of uncomplicated appendicitis. The sequence is typical: periumbilical or epigastric reference of pain at onset, followed by a shift to the right lower quadrant after a few hours. Tenderness, muscle spasm and rebound tenderness do not become prominent until the pain has shifted. Anorexia, nausea and vomiting occur after the illness has commenced with pain. Sudden cessation of pain is often coincident with perforation of the appendix.
The pattern of manifestations is generally less firmly predictable in diverticulitis. The location of the pain depends on the site and extent of the diverticulitis. Increased abdominal pressure, as in defecation, aggravates the pain. Rectal bleeding occurs in one-fourth of patients.
Pylephlebitis and Liver Abscess. The manifestations of pylephlebitis include chills, fever, epigastric or right upper quadrant pain, nausea, vomiting, enlargement and tenderness of the liver, and sometimes splenomegaly.
Fever, the most common finding in liver abscess, may be accompanied by chills and sweats. The second most common finding is right upper quadrant pain. The pain is aching in nature, and tends to be localized either over the liver itself or over the epigastrium. It may radiate to the right shoulder when it is aggravated by respiration. Percussion of the liver is painful. Anorexia, nausea and vomiting are uncommon. The course of the disease is indolent with hepatic enlargement, weight loss, marked leukocytosis and prostration.
Subphrenic Abscess. Subphrenic abscess formation is usually an insidious process. The manifestations may be nonexistent, are usually non-specific and may be misleading. The findings are commonly those of an intra-thoracic rather than an intra-abdominal condition. Dyspnea, cough, chest and shoulder pain and dullness or rales over the lung base may be noted.
Pelvic abscess. The symptoms of pelvic abscess are pain, deep tenderness in one or both lower quadrants, fever, urinary frequency, dysuria and diarrhea with passage of mucous in the first stools. Rectal or vaginal examination may reveal tenderness of the pelvic peritoneum and bulging of the anterior rectal wall. There may be fever, malaise, anorexia, or partial obstruction of the small intestine.
Pancreatic abscess. Acute pancreatitis is
classically manifested by severe epigastric pain that may be referred to
the back. The pain may be mild and short-lived or the attack may be fulminant,
with severe pain, hypotension and shock. There frequently is a history
of recent heavy ingestion of food and alcohol. Nausea and vomiting are
common. There is usually tenderness in the epigastrium, but this is absent
in early disease. Leukocytosis is present.
DIAGNOSIS:
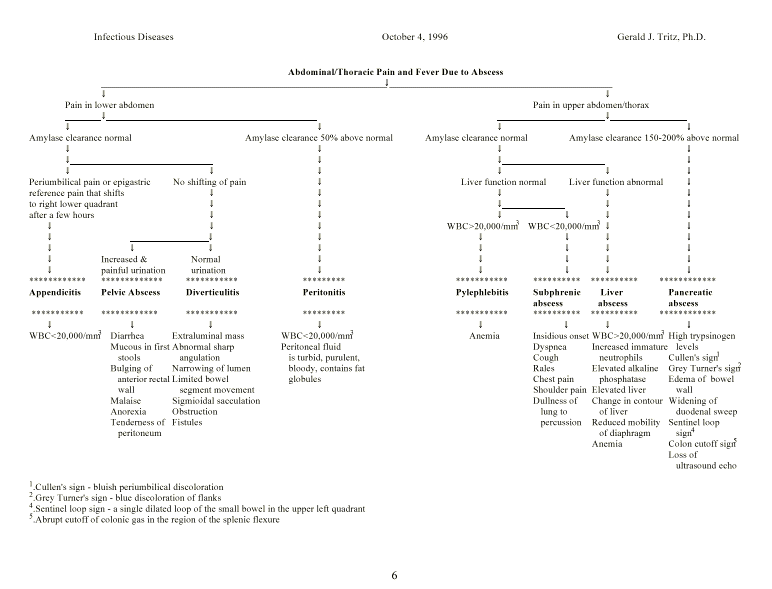
A differential diagnosis of the various anatomical
types of abscesses is based upon type and location of pain, white blood
cell count, biochemistries, imaging procedures and some pathognomonic signs.
Imaging procedures include X-ray, computerized tomography, positron emission
tomography, ultrasound and radioisotope imaging with gallium or indium.
TREATMENT:
The principles of therapy are:
1. To improve vascular perfusion by correcting fluid and electrolyte deficits
2. To combat the effects of bacteria and their toxic metabolites
3. To reduce paralytic ileus
4. To eliminate the primary source of infection by means of excision, closure or isolation
5. To aspirate infected exudate and to drain the site of the primary lesion
6. To treat local or distant complications as necessary
|
|
|
|