ID 1382-1406
OSTEOMYELITIS
OVERVIEW:
Most osteomyelitis is of
hematogenous origin. The clinical picture varies with age. In children
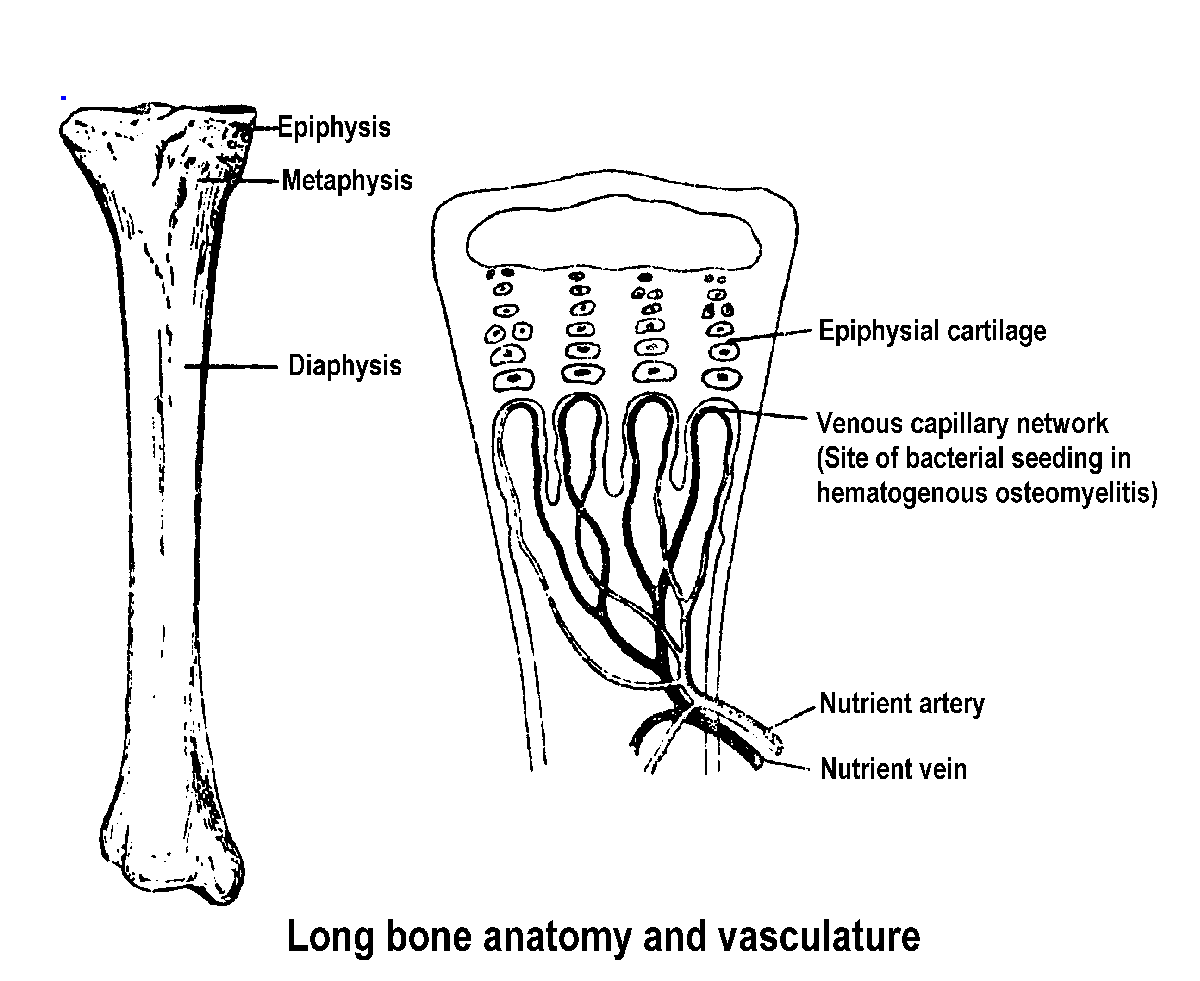
through the age of puberty the long bones of the extremities are most often
involved with the metaphysis as the initial infected site. In adults hematogenous
osteomyelitis most often affects the spine. This age-dependent preference
for bone relates to the vasculature and blood flow to the site. In children,
the metaphysis is very active metabolic tissue with a large blood flow
and with vasculature predisposed to infection. Phagocytes lining the capillaries
in this region are deficient in number and function. The nutrient arteries
near the epiphyseal cartilage are nonanastomosing, thereby allowing any
blockage to produce tissue necrosis and the sinusoids (venous side of capillary)
have slow, turbulent flow predisposing to thrombosis. As aging occurs metaphysis
metabolism slows down, blood flow decreases and phagocytic activity increases.
Concomitant with these changes the vertebrae become more vascular with
maturation (senile hyperemia) and bacteremias seed vertebral bodies preferentially
at the more vascular anterior vertebral end plates. In addition, lumbar
paracentral veins communicate freely with pelvic veins by valveless anastomoses.
Theoretically, retrograde flow from pelvic tissues (urethra, prostate,
bladder) to lumbar vertebrae explains the spread of pelvic infections preferentially
to lumbar vertebrae.
In about 25% of patients with osteomyelitis, the predisposing factor is trauma to the bone at or near the site of infection. Infections of the mandible are often due to traumatic dental procedures while the installation of prosthetic devices, such as artificial joints, predisposes to long bone infection.
ETIOLOGY:
Osteomyelitis is a purulent
inflammation of bone caused most often by bacteria and only occasionally
by other microorganisms. In order of frequency of infection the bacterial
species are:
Staphylococcus aureus )
Streptococcus spp. ) Long bone and spine infections
Members of the Enterobacteriaceae
)
Bacteroides spp. -
mandibular infections
PATHOLOGY:
The host responds to the
presence of bacteria in the metaphysis with a local increase in vascular
permeability, resulting in edema, increased vascularity and the influx
of polymorphonuclear leukocytes. Pressure increases as pus collects and
is confined within rigid bone. Exudation through Volkmann's canals and
the haversian canal affords little relief, although the relatively inelastic
periosteum may become elevated. The blood supply to the area of involvement
is decreased secondary to the pressure; necrosis of the infected bone may
result in the formation of a sequestrum. A protein-rich liquid containing
inflammatory cells may collect in an adjacent joint but such effusions
are sterile.
After the vascular supply
to the involved area has been interrupted and necrosis has occurred, the
chronic phase of osteomyelitis is established. The residual dead bone acts
as a foreign body, making the eradication of bacteria impossible until
the sequestrum is removed.
If the infected area becomes
well demarcated and the infection is contained, the acute inflammatory
process may subside, leaving a subperiosteal accumulation of pus which
may be discovered by tenderness on palpation. This relatively quiescent
form of subperiosteal infection is termed a Brodie's abscess.
After some time, there is deposition of new bone, the involucrum,
under the elevated periosteum.
In osteomyelitis of the spine,
infection most often involves the vertebral body. It spreads readily through
the anastomotic venous system to adjacent ligaments and vertebral bodies.
It is common for more than one vertebral body to be involved. Pus may accumulate
between the vertebral periosteum and dura mater, forming an extradural
abscess. Compression of the spinal cord may result, yielding a paraplegia.
If a subdural abscess ruptures into the subarachnoid space, meningitis
results.
CLINICAL SYMPTOMS:
Hematogenous osteomyelitis
is often preceded by the signs and symptoms of bacteremia:
Fever Inflammation
Malaise Cephalgia
Myalgia Anorexia
This phase of the illness
may last for several days.
The second phase of the disease
is the clinical onset of involvement of bone. This gives rise to:
Restricted motion
Pseudoparalysis
Soft tissue around the inflamed bone which is
Hyperemic
Warm
Edematous
Tender
Bone tenderness
DIAGNOSIS:
Diagnosis is based upon:
Clinical symptoms of an infection
Laboratory evidence of an infection:
Isolation of an organism
Increase in antibody titer
Presence of bone pain
Soft tissue swelling
Limited motion of extremity
Roentgenographic changes occur late in disease and should not be waited for to make the diagnosis; this would allow the development of chronic osteomyelitis. A differential diagnosis should include:
Rheumatic fever - there is severe pain and limitation of joint motion in this disease but there is no bone tenderness.
Monoarthritic rheumatoid arthritis - the major swelling and tenderness is limited to the joint, without local tenderness on palpation over the adjacent metaphysis.
Poliomyelitis - tenderness of the bone in an apparently paralyzed extremity indicates osteomyelitis. There is no bone tenderness in polio.
Septic arthritis - joints are exquisitely tender and painful, whereas the swollen joint associated with osteomyelitis may be gently manipulated through a limited range of motion.
Bacterial cellulitis - there is warmth, erythema, pain and edema of the soft tissue but it is clearly demarcated whereas in osteomyelitis it is not clearly demarcated.
TREATMENT:
Acute osteomyelitis should be treated with a parenterally administered antibiotic based on the infecting organism:
Staphylococcus aureus - nafcillin
Streptococcus pyogenes - nafcillin
Gram-negative rods - ciprofloxacin
Bacteroides spp. - clindamycin
Chronic osteomyelitis requires
surgical procedures as well as antibiotic therapy. This includes full debridement
and excision of all dead bone and necrotic tissue (sequestrectomy).