MM 302-304; ID 1185-1194
NONINFLAMMATORY GASTROENTERITIS
-
FOOD TOXEMIA
NAME OF DISEASE:
Food poisoning
Food toxemia
Botulism
OVERVIEW:
Food poisoning is a toxemia associated with the ingestion of preformed microbial toxins. It is NOT an infection. Since the toxins are ingested preformed and no microbial growth within the human is required, symptomology occurs rapidly, usually within 2-12 hours. These toxins either affect the intestine (enterotoxin of C. perfringens) or the central nervous system (neurotoxin of C. botulinum) or both (S. aureus and B. cereus).
ETIOLOGICAL AGENTS:
Staphylococcus aureus (gram+, aerobic, coccus)
Bacillus cereus (gram+, aerobic, rod)
Clostridium perfringens
(gram+, anaerobic, rod)
Clostridium botulinum (gram+, anaerobic, rod)
S. aureus toxin -
5 distinct antigenic types labelled A, B, C, D, E. They are water-soluble,
low molecular weight proteins that are
heat stable (resist boiling
for 30 minutes). Their mode of action is unknown but they each cause an
enteric effect (diarrhea) and a neurologic effect (vomiting). All are exotoxins
produced by chromosomal genes.
B. cereus toxin - The spore germination process of B. cereus produces several exotoxins which have either an enteric or a neurologic effect but not both. The type of toxin produced is dependent on the type of food that the spore germinates in. In a high protein food (meat) the enterotoxin is formed. In a high carbohydrate food (rice, pasta) the neurotoxin is formed. The enterotoxins stimulate the adenyl cyclase - cyclic AMP system in intestinal epithelial cells and cause fluid accumulation in the intestine. The neurotoxins cause vomiting through an unknown mechanism.
C. perfringens toxin - A single heat-labile protein of 34000 molecular weight inhibits glucose transport in intestinal epithelial cells, damages the intestinal epithelium and causes protein loss into the intestinal lumen. This activity is maximal in the ileum and minimal in the duodenum.
C. botulinum toxin
- 8 distinct antigenic types labelled A, B, C1, C2,
D, E, F, G. Types A, B, E, F and G are coded by chromosomal genes. C1
and D are coded by phage genes that are lysogenic in C. botulinum.
Types A, B and E cause almost all human botulism. All toxins are proteins
of 150,000 molecular weight that prevent release of acetylcholine at the
neuro-muscular junction causing a flaccid paralysis.
PATHOLOGY:
There is no pathology associated
with S. aureus or B. cereus toxemia. Epithelial cell lysis
is a microscopic pathologic effect of C. perfringens toxemia; rarely,
with heavily contaminated foods, there is a diffuse, necrotizing enteritis
of the jejunum, ileum and colon. The pathology associated with C. botulinum
is minimum, inconsistent and non-diagnostic.
CLINICAL SYMPTOMS:
In cases of gastroenteritis it is important to differentiate toxemia from infectious diarrhea. The key features are the rapidity of onset of symptoms following ingestion of contaminated food or drink, the lack of fever and the absence of fecal leukocytes. All of the toxemias result in symptoms occurring within 12 hours of toxin ingestion as compared to an incubation period of 24-72 hours for infections.
S. aureus - Vomiting (often projectile) little or no diarrhea, no fever. Symptoms occur within 1-4 hours after ingestion of contaminated food (generally mayonnaise or dairy products).
B. cereus - Type 1: When the organism grows in starchy foods especially fried rice, there is emetic illness 2-3 hours after ingestion and a little diarrhea. No fever. Type 2: When the organism grows in meat or cream sauce or gravy there is profuse diarrhea with a little vomiting at 10-14 hours after ingestion. No fever.
C. perfringens - Abrupt onset of profuse diarrhea with little or no vomiting about 12 hours after ingestion of meat. No fever.
C. botulinum - Onset
of symptoms between 6 hours and 8 days after ingestion of green beans,
peppers, chili or sausage. The length of the incubation period is a function
of the amount and antigenic type of toxin ingested. The illness is characterized
by symmetric impairment of cranial nerves, followed in a descending pattern
by weakness or paralysis of the muscles of the extremities and trunk. All
symptomology is due to blockage of release of the neurotransmitter at the
neuro-neuro junction or the myoneuro junction. Common presenting signs
are:
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
On physical examination,
ophthalmoplegia and ptosis of the eyelids are usually prominent, along
with a decreased gag reflex and facial muscle weakness. Mental status and
deep tendon reflexes are normal. Electromyographic abnormalities are frequently
present, although a normal electromyogram does not rule out botulism. Characteristic
EMG findings include diminution of the amplitude of muscle action potentials
after a single supramaximal nerve stimulus and facilitation of the action
potential when paired stimuli are delivered at an interval of 2.5 msec.
Nerve conduction studies, blood cell counts, urinalysis, serum electrolytes,
cerebrospinal fluid and blood enzymes are normal. No fever.
DIAGNOSIS:
Since the only fatal toxemia in this group is botulism, the emphasis should be on ruling out botulism in the diagnosis. The other toxemias are not severe and symptoms generally disappear within 24 hours. In fact the physician is hardly ever consulted in the mild toxemias. Presumptive diagnosis of botulism is made by the presence of a rapidly descending paralysis. A history of ingestion of home canned food or honey is helpful. Confirmative diagnosis is made by demonstrating botulinal toxin in the patients serum or feces or in incriminated food using a mouse toxin-neutralization test. A differential diagnosis should include:
Guillain-Barré syndrome - this is an ascending paralysis. There is paresthesias or other sensory abnormalities and elevated cerebral spinal fluid protein. There may be a history of an antecedent viral infection.
Myasthenia gravis - this is a descending paralysis. There is accentuation of muscle fatigability during exercise and positive response to endrophomium
Other microbial food poisonings
and gastroenteritis - there is no cranial nerve involvement in these diseases
Chemical (non-microbial)
food poisonings - symptoms occur within minutes of ingestion
TREATMENT:
In toxemia due to S. aureus,B. cereus, C. perfringens the only treatment employed, and one used rarely, is replenishment of fluids and electrolytes. Patients with signs or symptoms compatible with botulism, or patients who are known to have eaten food shown by laboratory testing to contain botulinal toxin, should be admitted to an intensive care unit to permit monitoring of respiratory and cardiac function. Airway patency should be guaranteed by insertion of an endotracheal tube or tracheostomy before bulbar or respiratory impairment becomes severe. Induction of vomiting or gastric lavage is recommended if exposure has occurred within several hours. Unless there is paralytic ileus, purgation is advisable, even after several days, to facilitate possible elimination of unabsorbed toxin from the gastrointestinal tract; alternately, high enemas may be used.
Injectable therapeutics sometimes used include:
1. Trivalent (ABE) equine-origin botulinal antitoxin to neutralize unabsorbed toxin.
2. Guanidine hydrochloride to increase release of acetylcholine from nerve terminals.
3. 4-Aminopyridine
to increase release of acetylcholine.
INFANT BOTULISM - A SPECIAL CASE
Several years ago it was
recognized the C. botulinum could colonize the gastrointestinal
tract of the infant. C. botulinum spores in honey used to sweeten
infants milk or water, when ingested, geminate in the infants intestinal
tract, colonize it and produce toxin in vivo. Constipation is the
first sign of disease; this is followed by the same neurological signs
seen in the adult. Antibiotics are generally not effective and may exacerbate
the illness by elimination of normal flora. Therapy is the same as for
adult botulism except that antitoxin is generally not used because the
disease is milder in children.
MUSHROOM POISONING
The ingestion of fleshy fungi (mushrooms) can be a gourmet's delight or a harbinger of various side effects ranging from mild gastrointestinal distress to hallucination to delirium to coma to death. There is no simple way to separate the majority of mushrooms into those that are delectable and those that are poisonous. Mushroom poisonings are classified according to the organ system exhibiting major involvement.
Mycetismus gastrointestinalis
When the gastrointestinal tract shows major involvement, there may be mild discomfort or violent retching and diarrhea accompanied by cramps. The water loss may be great and cause subsequent electrolyte imbalance. Sometimes there may be cerebral manifestations, with dizziness and slight hallucination. Treatment is not usually necessary although gastric lavage may be helpful.
Mycetismus choleriformis
When the ingested mushrooms affect the activity or concentration of acetylcholine there is a severe and frequently fatal illness. The major feature of this form of disease is a long symptomless period (6-24 hours) following ingestion. The symptoms begin suddenly and are characterized by violent vomiting, continuous diarrhea, dehydration and muscle cramps. Fluid loss amounts to 2-3 liters per day. There is a feeble rapid pulse. No sensory loss is noted at this stage but the patient may be listless and apathetic. The poisoning is distinctly diphasic. Symptomatic treatment results in remission; however, there is often a fatal relapse. The terminal symptoms include a sudden onset of confusion, coma, sweating, miosis, muscular twitching, lacrimation and salivation. This is due to the action of the toxins amanitine and muscarine on smooth muscles and exocrine glands innervated by the cholinergic nerves. Treatment is large doses of atropine.
Mycetismus nervosus
When mushroom poisoning affects
the parasympathetic nervous system and the gastrointestinal tract within
two hours of ingestion, the symptoms are due to muscarine only.
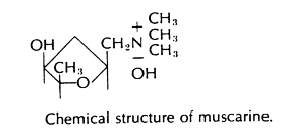
There is violent gastrointestinal involvement, profuse sweating, convulsions, contracted pupils and salivation. Depending on the dose of the toxin, the patient develops delirium, hallucination or coma. Death may result if sufficient toxin is present and is due to cardiac and respiratory failure. Atropine administration is the preferred treatment.
Mycetismus sanguinareus
When the ingested toxin destroys the red blood cells, the result is hemoglobinuria and transient jaundice six to eight hours after ingestion of raw or under cooked false morel mushrooms (Helvella esculata) The toxin that causes this is monomethyl hydrazine. Treatment is not usually necessary.
Mycetismus cerebralis
When the ingested toxin causes hallucinations, it is generally due to the hallucinogen, psilocybin.
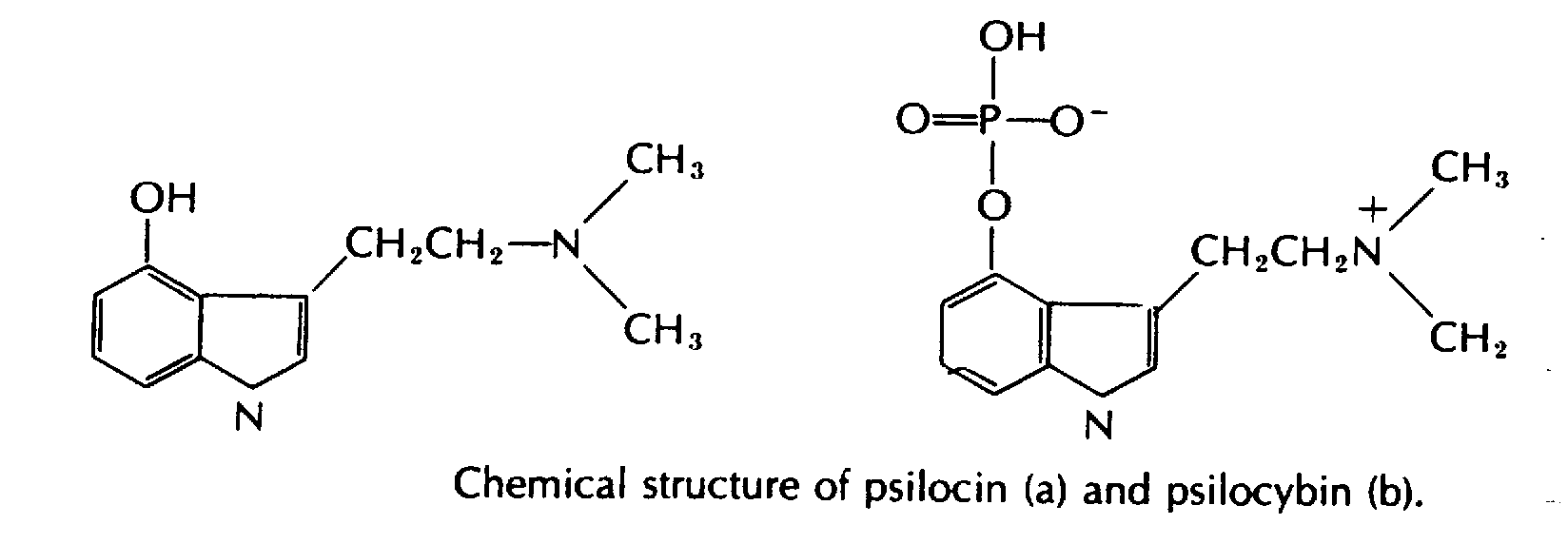
This is found in several
species of mushroom of the genus Psilocybe.